It’s rare, but in a population as big as the United States, myocarditis, which is inflammation of the heart muscle, still affects millions of Americans every single year. In 2017 alone, 3.1 million cases of myocarditis were professionally diagnosed. The danger with myocarditis is its relative obscurity.
The cause of the disease often eludes the professionals in charge of treating it, and its symptoms can sometimes be imperceptible. More than that, most of us barely know a thing about this serious condition. So, in an effort to better understand it, let’s uncover the symptoms, causes, and treatment options for myocarditis.
Myocarditis and Inflammation
Many of us are already aware of the dangers of inflammation and the benefits of being proactive. Inflammation can wreak havoc on your immune system and stand in the way of the things that you love to do.
Your myocardium, or the muscle layer of your heart, isn’t out of reach of the destructive impact of inflammation either. In fact, inflammation plays a central role in today’s featured condition.
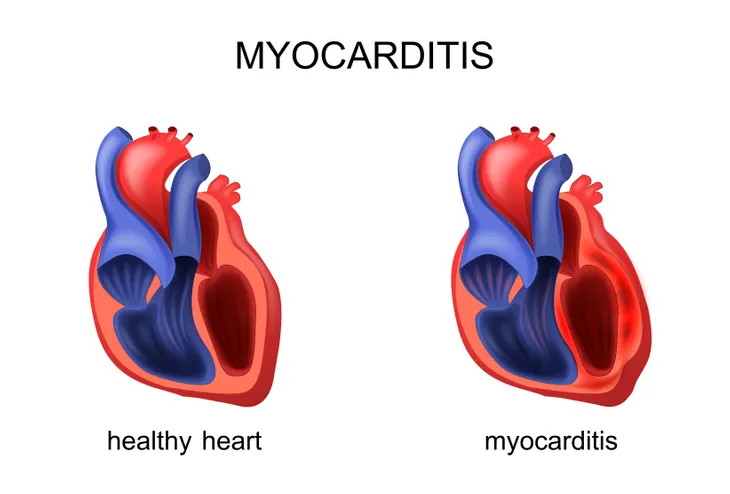
What Is Myocarditis?
Myocarditis causes inflammation of the muscle layer of the heart. This inflammation can cause the heart to enlarge and weaken, create scar tissue, and restrict its ability to circulate blood and oxygen throughout the body.
This inflammation of the heart often leads to a collection of symptoms, both large and small, and can dramatically impact your overall health and wellbeing. Next, we’ll look at some of the most common symptoms of myocarditis.
Symptoms of Myocarditis
The inflammation caused by myocarditis can negatively impact all elements of your life. Your heart is inarguably one of the most important organs in your body, so it shouldn’t surprise anyone. Although, the sheer variety of symptoms can make diagnosing myocarditis difficult.
Symptoms of myocarditis may include shortness of breath, fatigue, heart palpitations, chest pain or pressure, lightheadedness, swelling in the hands, legs, ankles, and feet, and even a sudden loss of consciousness.
When to See a Doctor
Should you experience any of the previously mentioned symptoms, however faintly, reaching out for professional help is paramount.
Although mild cases of myocarditis often improve on their own, medication and surgical intervention may be required (but more on that later). Up next, let’s look at what we know about the causes behind myocarditis.
Myocarditis Causes
As previously stated, a lot of cases of myocarditis are never associated with an outright cause.
The cases that are sourced to a root cause are typically attributed to a variety of viral infections that have made their way to the heart muscle. Let’s take a closer look at some of the possible causes.
Viruses and Bacteria
Viruses are the most frequent cause of myocarditis. The most common virus culprits include coxsackievirus group B, human herpesvirus 6, and parvovirus B19. Also, Epstein-Barr virus and rubella virus have also been linked to myocarditis in the past.
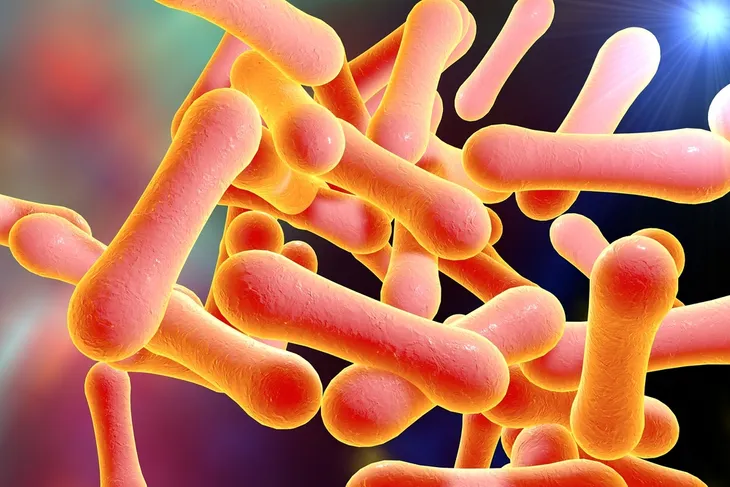
Bacteria have also been linked to myocarditis. Staphylococcus aureus or Corynebacterium diphtheriae are the most prominent myocarditis-linked bacteria.
Fungi and Parasites
Fungi, sourced from yeast infections, or interactions with various molds can also lead to the development of myocarditis.
Finally, though rare in the United States, parasites, or microorganisms that feed off other organisms, have been shown to cause myocarditis in Central and South America.
Diagnosing Myocarditis
If you’ve noticed the appearance of one or more of the symptoms above, book an appointment with your doctor immediately.
To diagnose myocarditis, your doctor may suggest a chest X-ray to see if there’s been any cardiac enlargement. For the same reason, your doctor may request an electrocardiogram (ECG), which is a medical test that can detect some heart abnormalities.
Treatment: Medicine
If you do in fact have myocarditis, your doctor will set out to treat its cause, whether that be viral, bacterial, or any number of the established causes.
Your doctor may also prescribe medicines designed to help your heart work better. Examples of these types of medications include angiotensin-converting enzyme (ACE) inhibitors, beta-blockers, and diuretics.
Treatment: Lifestyle Changes
Once you’ve been assessed and prescribed the necessary medications, your doctor will most likely insist on a few lifestyle changes. A prolonged period of rest and reduced activity will likely be recommended. You may also be encouraged to maintain a low-salt diet.
Keep in mind if you experience complications from myocarditis, such as a weakened heart or a blood clot, you may need to be hospitalized. Furthermore, if you experience a severe abnormal heartbeat (termed an arrhythmia), you may need other medications or even an implantable cardioverter-defibrillator (ICD) or a pacemaker.
Outlook
Your outlook relies on a few factors including the cause of your myocarditis, the state of your overall health, and if you have any complications.
The good news is, many people can recover completely. However, in some cases, it can be a chronic condition. This is even more reason to seek immediate medical help as soon as symptoms begin to occur.
Possible Risks
It’s vital that you receive treatment if you suspect you have myocarditis. If left untreated, it may lead to serious complications such as heart failure.
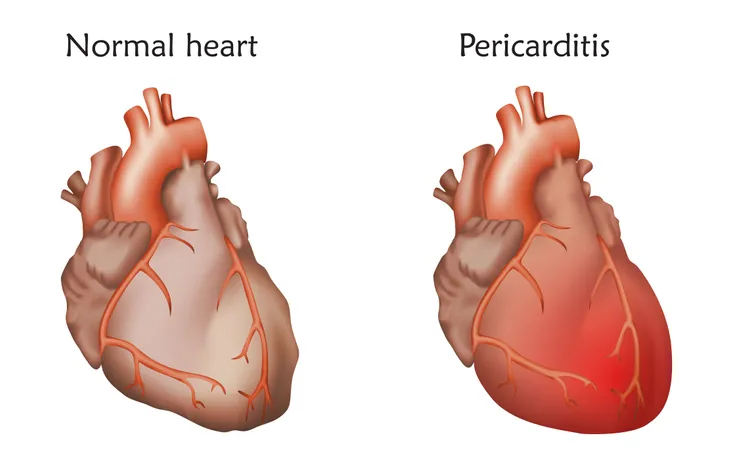
In rare cases, it may lead to cardiomyopathy which means the heart muscle weakens or the structure of the heart changes. It could also lead to pericarditis, which means the sac that covers the heart becomes inflamed.
Prevention
As you’ve just learned, myocarditis should be approached with the utmost caution. Sure, it has been known to clear up on its own in the past, but if left untreated, the buildup of scar tissue can leave you with lingering health effects for the rest of your life.
Being proactive today may not protect you from myocarditis outright, but talking to your doctor as soon as possible may help you avoid a serious complication later. Staying up to date with vaccinations, avoiding ticks, and maintaining proper hygiene can protect you from the various viruses, bacteria, fungi, and parasites that cause myocarditis.