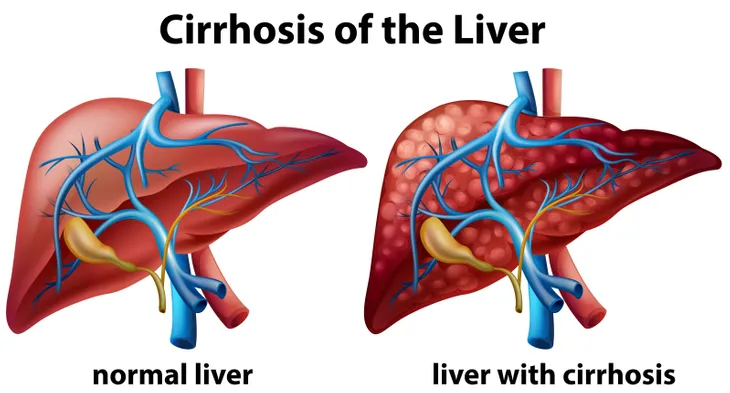
Liver cirrhosis is a serious condition in which healthy liver cells are replaced by scar tissue. According to MedicalNewsToday.com, “It is a progressive disease, developing slowly over many years,” that most often presents in the late stages of chronic liver disease.
Cirrhosis occurs as a result of long-term damage to the liver. Over the years, as the liver becomes more damaged, scar tissue forms as the body tries to repair the organ. This repeated damage leads to a build-up of scarring, which “can start blocking the flow of blood through the liver,” eventually causing it to stop functioning altogether, if left untreated, says the source. Read on to learn more about the causes and symptoms associated with liver cirrhosis, as well as how it can be treated with these 12 facts.
Cause: Chronic Alcohol Abuse
There are a wide variety of different diseases and conditions that can cause damage to the liver over time, eventually leading to cirrhosis. Among the most common, however, is chronic alcohol abuse. Overconsumption of alcohol over a prolonged period of time can cause inflammation and fat to build up in the organ.
While WebMD says, “The amount of alcohol it takes to hurt the liver is different for everyone,” generally speaking, women should limit their consumption to one drink per day and men should limit their consumption to two drinks per day. Although not everyone who consumes more than this amount of alcohol each day will get cirrhosis, it certainly puts them at increased risk.
Cause: Chronic Viral Hepatitis
Another primary cause of liver cirrhosis is hepatitis, which is defined as inflammation of the liver. In some cases, hepatitis may be caused by taking certain medications or abusing alcohol, but it most often occurs because of a virus (e.g., the hepatitis B virus [HBV] or hepatitis C virus [HCV]).
Hepatitis B and C are the most common types and, are usually contracted by exposure to infected blood. This can occur through sexual intercourse or if you come into contact with contaminated needles, as well as when you are tattooed, pierced, or taking drugs intravenously. Hepatitis D can also cause liver cirrhosis, but this type of hepatitis can only develop in those who already have contracted hepatitis B.
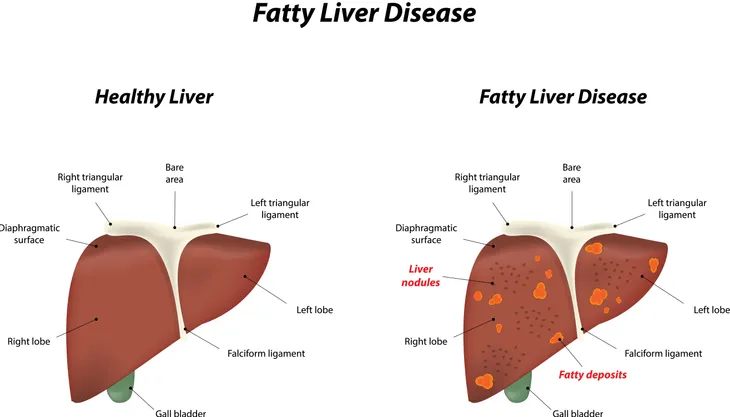
Cause: Nonalcoholic Fatty Liver Disease
As mentioned earlier, alcohol abuse can cause fat to build up in the liver, which may eventually lead to cirrhosis. But in some cases, this fat build-up occurs even if you don’t drink alcohol, as a result of other conditions. This is referred to as non-alcoholic fatty liver disease or steatohepatitis.
The diseases that are most commonly linked to non-alcoholic fatty liver disease include diabetes and coronary artery disease, but it can also occur as a result of conditions such as obesity, having high blood cholesterol, or high blood pressure.
Other Causes
While the above mentioned conditions are considered the primary causes of liver cirrhosis, they’re certainly not the only factors that can cause it. Other factors include genetic conditions like hemochromatosis, where iron builds up in the body, and Wilson’s disease, where copper accumulates in the liver and elsewhere in the body.
Liver cirrhosis may also occur if the bile ducts become blocked, such as with cancer, or damaged, which can occur with gallstones or cystic fibrosis. Taking certain medications—both over-the-counter and prescription—can also cause cirrhosis, including “acetaminophen, some antibiotics, and some antidepressants,” says Healthline.com.
Stages
Liver cirrhosis occurs in two stages: compensated and decompensated. With compensated, you won’t experience any symptoms. WebMD explains that this is because “there are still enough healthy liver cells to meet your body’s needs. They compensate, or make up for, the damaged cells and scarred tissue.”
Without treating the underlying cause, however, the cirrhosis will progress, and eventually “the healthy liver cells won’t be able to keep up,” according to the source. When this happens, it is referred to as decompensated cirrhosis, and you will start to experience a variety of symptoms (which we’ll discuss next).
Symptoms
There are a wide variety of symptoms that can occur with decompensated liver cirrhosis. These include loss of appetite, bleeding and bruising easily, itchy skin, weight loss, and yellow discoloration of the skin and eyes (known as jaundice).
As the cirrhosis worsens, more serious symptoms may present themselves. For instance, you may become confused, have difficulty thinking clearly, and slur your speech. Alternatively, you may begin to accumulate fluid in your abdomen, which is known as ascites, and men with cirrhosis may also develop enlarged breasts (gynecomastia) and struggle with impotence.
Diagnosis: Lab Tests
If you notice yourself experiencing any of the symptoms previously mentioned, it’s important to make an appointment with your doctor to obtain a diagnosis. There are many different ways a medical professional may go about this, the first of which is through conducting lab tests.
To check liver function, for instance, a blood sample is taken and “checked for excess bilirubin, which is a product of red blood cells breaking down, as well as for certain enzymes that may indicate liver damage,” says the Mayo Clinic. A blood sample may also be taken to test for the hepatitis virus, the blood’s ability to clot and kidney function, which the source says can decline as cirrhosis progresses.
Diagnosis: Other
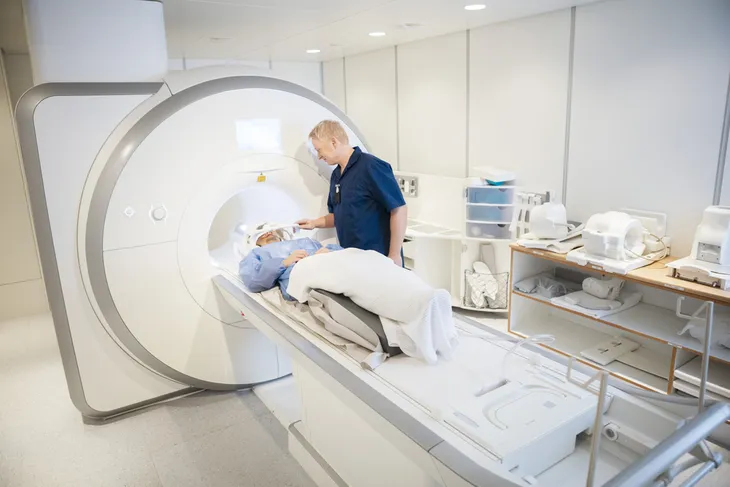
In addition to blood tests, your physician may order other types of tests to help with diagnosis. These include imaging tests, such as magnetic resonance elastography or transient elastography, which “detect hardening or stiffening of the liver,” says the Mayo Clinic. Other imaging tests such as MRI, CT, and ultrasound, may also be conducted.
In some cases, a liver tissue sample (biopsy) may be helpful as well. Although the source says it’s not necessary for a diagnosis, “your doctor may use it to identify the severity, extent and cause of liver damage.”
Treatment: Underlying Causes
Treatment for liver cirrhosis is dependent on the underlying cause of the condition, as well as how far it has progressed. If cirrhosis is occurring because of alcohol abuse, it’s important that people cease consumption. This may not always be easy, however, due to long-term dependency, in which case a treatment program may be necessary.
If hepatitis is the cause, medications may be prescribed in order to limit the liver damage caused by these viruses. Also, if cirrhosis is being caused by nonalcoholic fatty liver disease, people may find losing weight and controlling their blood sugar levels to be effective treatments.
Treatment: Complications
There are many different complications that can occur as a result of having liver cirrhosis. One of the most common is portal hypertension, which is high blood pressure in the vein that supplies the liver with blood. Other complications include fluid retention (causing edema and ascites), and increased susceptibility to infections.
To help treat portal hypertension, for instance, blood pressure medications may be prescribed. Also, with excess fluid build-up, a low-sodium diet along with medications may be effective in reducing swelling. If you have an infection, your doctor may prescribe antibiotics. To help prevent future infections, however, they may recommend you get vaccinated for common illnesses such as the flu, pneumonia, and hepatitis.
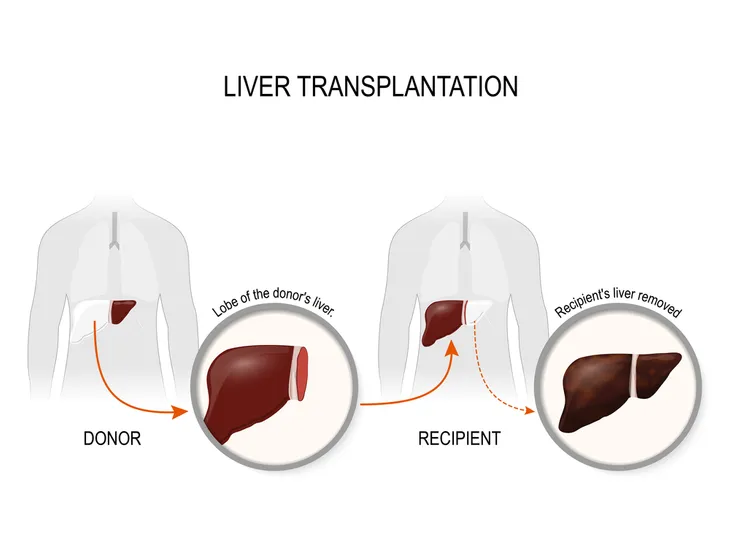
Treatment: Liver Transplant
When cirrhosis reaches an advanced state, and the liver stops functioning, receiving a new liver via transplant is the only treatment option. According to the Mayo Clinic, this process “replaces your liver with a healthy liver from a deceased donor or with part of a liver from a living donor.”
A transplant is considered a last resort, however, as it can take a great deal of time to find a donor. Also, the affected individual has to “undergo extensive testing to determine whether they are healthy enough to have a good outcome following surgery,” says the clinic.
Prevention
Fortunately, liver cirrhosis can be prevented altogether by being aware of behaviors and factors that can increase risk. When it comes to alcohol, for example, it’s important to drink in moderation and be mindful of daily and weekly limits.
You can reduce your risk of contracting hepatitis by practicing safe sex, not sharing needles, and getting vaccines to protect against these viruses. Additionally, preventing fat build-up in the liver requires eating a healthy, balanced diet that contains plenty of fruits and vegetables, whole grains, and lean proteins in order to maintain a healthy weight.