Night sweats is an uncomfortable occurrence, but can actually be quite common. Night sweats refer to any type of excess perspiration or sweating at night. In many cases night sweats aren’t attributed to wearing too many blankets or the balmy temperature in your bedroom, but rather an underlying medical condition.
In most cases, night sweats are not a serious symptom, but if it occurs on a regular basis, it may be helpful to assess what may be triggering it. If you’re struggling with night sweats, there are a variety of common medical causes that could be beneficial to be aware of. Here are 12 common medical causes of night sweats.
1. Menopause
If you’re female, and at a certain ripe age, your night sweating may be contributed to menopause or perimenopause. Cleveland Clinic explains that night sweats are the nocturnal counterpart to hot flashes, and are common during the menopausal transition as hormone levels change. When you experience night sweats because of menopause, you may wake up feeling cold and your sheets could be soaked from your sweat. In addition to this unfortunate scenario, your heart may also be pounding. To help cope with these symptoms, set your temperature lower at night, use low thread count sheets (the higher the thread, the less they breathe), and try some deep breathing exercises before bed and when you wake up from the sweats.
Waking up in the middle of the night is bad enough without the cold sweats, and it can be difficult to get back to sleep because of it. While menopausal or premenopausal women can experience this, men, younger women and children can also get night sweats due to hormonal imbalance if they suffer from pheochromocytoma, an adrenal gland disorder.
2. Certain Medications
Night sweating is often a side effect of prescription medications. For example, medications to treat depression, such as tricyclic antidepressants and selective serotonin reuptake inhibitors (SSRIs), often cause night sweats. In addition to antidepressants, the Mayo Clinic indicates that hormone therapy medication and drugs that lower your blood sugar level can cause night sweats too.
There are also some medications or treatments you may find surprising that can cause night sweats, such as cortisone. Cortisone is a steroid that reduces inflammation and relieves pain, and is administered through a needle. It’s used to treat several diseases and health problems, from carpal tunnel and variations of arthritis to gout and lupus. Make sure you tell your doctor if you experience anything new like night sweats shortly after starting new medications – it could be a side effect. You and your doctor may need to experiment with a few different options to find the right fit.
 Shutterstock/fizkes
Shutterstock/fizkes3. Tuberculosis
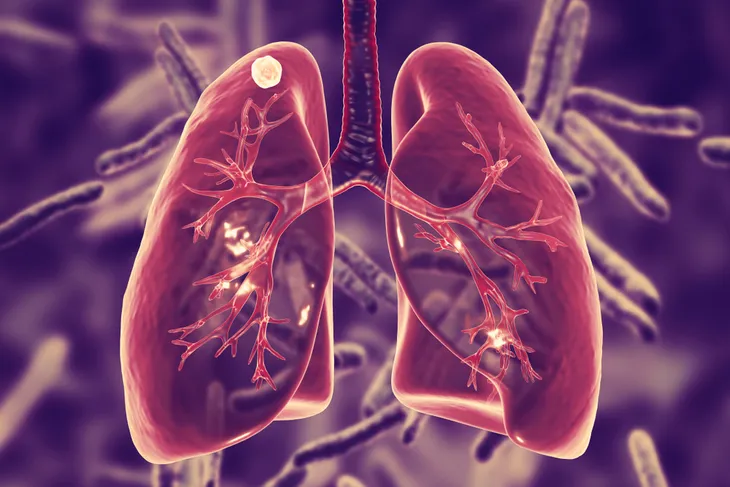
While night sweats can be caused by a number of issues that are easily fixed or managed, some are caused by serious illnesses and diseases like tuberculosis. In centuries past, tuberculosis was the most common cause of night sweats. This potentially fatal and highly contagious disease most commonly infected the lungs and caused severe night sweats.
Night sweats are a mild symptom of tuberculosis usually brought on by an accompanying fever. Other symptoms can be much worse, including coughing up blood, chest pain, trouble breathing, and a high fever. On top of this, according to the Mayo Clinic, tuberculosis can also affect your kidneys, spine and brain. The way the disease affects these other areas of your body varies. The number of TB cases and deaths in the U.S. has drastically decreased over the years, but there are other areas in the world where the disease is still wreaking havoc, causing an estimated 1.5 million deaths this year.
4. Abscesses
Bacterial infections, such as serious abscesses—including appendix, boils, tonsils, and diverticulitis flare-ups—are all common sources of night sweating as the body tries to fight off the source of infection. Night chills and sweats from abscesses are usually accompanied by a fever. These pus-filled infections can be extremely painful and can swell and grow to be very large.
There are two types of abscesses, skin and internal. Skin abscesses grow under the skin, and are much easier to identify than internal abscesses because you can see the infection and the area it’s affecting. Many skin abscesses naturally go away but in some cases, an antibiotic may be required. Or, your doctor may have to drain the infection by making a small incision over the swollen area. But internal abscesses can take longer to diagnose. The patient will have pain in the general area of the infection, may get a fever, and generally feel sick. These internal abscesses often develop as a complication from a pre-existing condition.
 H_Ko / Shutterstock
H_Ko / Shutterstock5. HIV and AIDS
Those infected with HIV or who have AIDS could experience nocturnal sweating so severe and profuse that bedclothes, sheets, and blankets are entirely saturated and soaking with perspiration upon waking. While night sweats aren’t always a sign of infection, those who are living with HIV are at a higher risk of infection, and those infections can be quite serious. General night sweats are uncomfortable, but if there’s a fever present as well, it’s likely a sign of infection.
Healthline explains that in the first couple weeks of being infected with HIV, a lot of people will have flu-like symptoms, including night sweats. As the virus settles into the body, the body’s natural response is to fight back, resulting in various forms of sickness. Chills and rashes could also occur during this phase. It’s important to consult your doctor if you were or are at risk of exposure and experience new night sweats or flu-like symptoms.
6. Low Grade Migraine Medication
WebMD explains that something as simple as aspirin or acetaminophen, taken to treat a severe headache or low grade fever will often result in night sweating, as well as a flushing or reddening of the skin on the neck and face. Make sure you follow the instructions on the label about how much you can take and how often. Never increase your dosage above the recommendations unless your doctor has told you to do so.
You might be able to prevent or decrease the severity of night sweats that are a result of taking low grade pain medication by alternating the type of medication you take. Instead of taking the recommended dose every 4-6 hours (or whatever it specifies on the label), take a different type of pain reliever when it’s time for another dose, and switch back and forth. This might help reduce your night sweats. Of course, you should talk to your doctor about doing this beforehand, and if you require regular medication for headaches or fevers, there might be a medical condition causing them. Other medications you’re taking could cause a bad interaction with the pain medication, leading to night sweats too.
7. Cancer
Nocturnal perspiration is also an early warning sign of certain types of cancer, the most common being lymphoma, a form of cancer that attacks the cells of the lymphatic system. The profuse night sweating is often accompanied by fever, and severe and drastic weight loss. Sweating could happen during the day too, depending on the cause and situation.
While night sweating can be a warning sign of cancer, it may also be caused by cancer treatments. According to the National Cancer Institute, several types of cancer treatments can result in night sweats and hot flashes, including hormone therapy, chemotherapy, radiation, and drugs to prevent or manage cancer. Common drugs that cause sweating are Tamoxifen, aromatase inhibitors, opioids, tricyclic antidepressants, and steroids. It can be uncomfortable and embarrassing when you sweat a lot, but this side effect is often not considered severe or a significant health risk. It’s always best to let your physician know any side effects you experience from your cancer treatment.
8. Neurologic Issues
Sweating is a normal, natural function to manage the temperature of your body and to cool it down when it’s hot. Healthline explains that night sweats may also be a reaction when you’re nervous or anxious, but sometimes sweating at night can be caused by a medical condition. Common neurologic conditions—such as stroke and autonomic neuropathy, and Parkinson’s disease—can make patients prone to night sweats. Since sweating is related to your nerves and how they function, the damaged nerves caused by many of these neurological conditions will result in faulty signals sent to the sweat glands, causing them to overwork and cause profuse nocturnal sweating.
It’s actually not very common for night sweats to be a result of neurologic issues, but it is possible for some people and situations. Tracking how often you wake up drenched in sweat, as well as other symptoms that you’ve recently started to experience will help your doctor find the cause. Although it’s not common from neurologic conditions, these conditions can be quite serious and should be investigated. Go to your doctor so they can find the underlying cause.
9. Chronic Hyperhidrosis
Idiopathic hyperhidrosis, or excessive sweating, is actually a medical condition characterized by the body’s production of excess sweat. This is considered a chronic condition although no concrete medical cause is linked to it other than genetics or family history. People with this condition sweat easily and often. What a regular person without the condition considers a cool temperature, people with idiopathic hyperhidrosis could feel it’s too hot or sweat regardless of the temperature.
Healthline explains that hyperhidrosis isn’t a serious threat to your health, but it can be uncomfortable and embarrassing when the person can’t control or prevent themselves from sweating. That said, some people sweat a lot because they have an underlying cause that could be serious. Doctors often refer to this as secondary hyperhidrosis. If there isn’t a medical condition or medication causing you to sweat, there are a few things that may help reduce excessive sweating, including prescription antiperspirants and lifestyle changes.
10. Hypoglycemia
Those who suffer from hypoglycemia, a condition that causes low blood glucose levels, may experience night sweats both in the pre-diagnosed stage and in the after stages. The drop in blood sugar levels over night can lead you to sweat profusely, and can sometimes result it nightmares and headaches. On top of low blood sugar causing night sweats, many medications prescribed to treat hypoglycemia can cause night sweating as a side effect as well.
Hypoglycemia can interfere with the way your nerves function, which is called autonomic neuropathy, (previously explained in this article). The damaged nerves don’t send the proper signals to your sweat glands, resulting in night sweats. People who have an autonomic neuropathy condition and hypoglycemia are likely to sweat more easily from certain foods and during light exercise. For people with diabetes who struggle with high blood sugar, the medication to lower your blood sugar could make you hypoglycemic at night, resulting in night sweats and anxiety. If this happens, talk to your doctor about your options to prevent or reduce the amount you sweat.
 Shutterstock
Shutterstock11. Sleep Apnea
The sleep disorder sleep apnea is another possible underlying medical condition that could be causing your night sweats. Healthline explains that sleep apnea is a condition that stops you from breathing multiple times a night while asleep. Those with obstructive sleep apnea tend to relax their throat muscles when they sleep, which they shouldn’t and can interfered with the airways ability to transport air to and from the lungs.
A few common side of effects of sleep apnea include loud snoring, dry mouth, morning headache, abrupt awakening, and night sweats. If you feel that you may be struggling with night sweats due to sleep apnea, it may be time to seek the help of your doctor or a sleep specialist to determine treatment.
12. Anxiety Disorders
While anxiety is a mental health disorder, it can also cause physical symptoms, including night sweats. It’s best to consult a therapist to address the underlying cause of your anxiety and seek coping mechanisms to live a happy, healthy lifestyle. A few other common physical symptoms of anxiety include muscle tension, a rapid heartbeat, difficulty breathing, and digestive issues.
Healthline explains that if you’re experiencing night sweats alongside anxiety, it may be a sign that your anxiety might not be as under control as it could be. If one of your symptoms of anxiety is night sweats, be sure to bring this up to a doctor. They can help you come up with a plan of action and may suggest treatments such as therapy, anti-anxiety medications, lifestyle changes, or a combination of methods.
 Shutterstock/WichM
Shutterstock/WichM