Type 1 diabetes causes the body’s immune system to destroy the beta cells in the pancreas which leads to an inadequate production of the hormone that regulates glucose in the blood. While glucose is required as a main source of energy, the buildup of glucose in the bloodstream can result in potentially life-threatening complications.
While there may be no proven cure or form of prevention just yet, below is an explanation of what tried and true forms of treatment are available to the over 1.25 million Americans dealing with type 1 diabetes every year.
Want diabetes content delivered straight to your inbox? Sign up for our Diabetes newsletter and receive exclusive news and articles written from our team of diabetes experts.
Taking Hormones
When the body can’t produce enough of the hormone that regulates glucose in the blood (this is what keeps blood sugar levels in a normal, healthy range), as is the case with diabetes, you have to provide your body with an external source of this hormone.
There are different kinds of this medication — all of which are used for different purposes and times of day, as prescribed by your doctor. The different kinds include:
- Short-acting (e.g., regular or novolin)
- Rapid-acting (e.g., lispro [Humalog]
- Intermediate-acting (e.g., NPH)
- Long-acting (e.g., glargine [Lantus])
Regardless of what kind of medication is prescribed, injecting the hormone into your body with a needle or pump (basically a small tube placed just under the skin that stays on your body) is the only way to effectively administer it.
With injections, most people require multiple daily injections that include a combination of a long-acting and rapid-acting to try to mimic the body’s normal use of the hormone. The number of shots required each day will be different from person to person and can change depending on the state of your diabetes as overseen by your doctor.
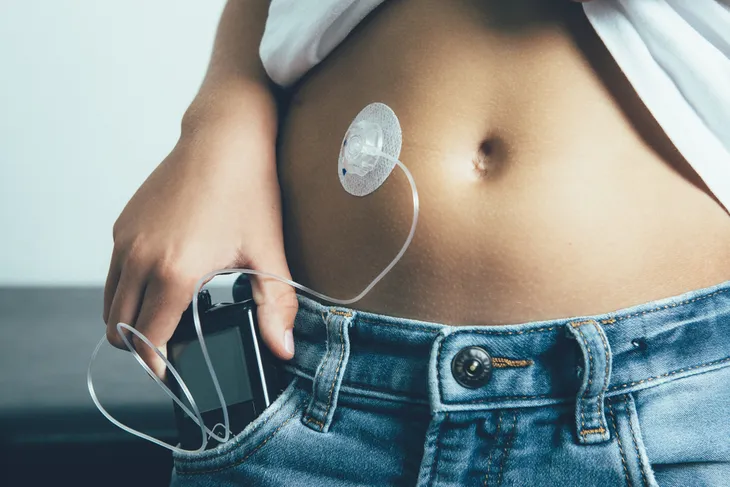
The pump, on the other hand, consists of a smartphone-sized device that is worn on the outside of the body with a tube that inserts under the skin of your abdomen.The tube will automatically administer specific amounts of the rapid-acting form of the hormone based on the meals you eat and your blood sugar levels throughout the day.
It’s important to note that this hormone can’t be taken orally. If taken orally, the hormone would break down in your intestines before it’s able to have any medicinal effect.
Taking Other Medications
Other than taking the hormone that allows the body to use glucose for energy, diabetics may be required to take additional medications to treat type 1 diabetes, including:
- High Blood Pressure Medications: Angiotensin-converting enzyme (ACE) inhibitors or angiotensin II receptor blockers (ARBs) are often prescribed to help keep kidneys healthy for people who have blood pressures above 140/90-millimeters of mercury (mm Hg).
- Cholesterol-Lowering Drugs: Due to people with diabetes having an elevated risk of heart disease, these drugs are prescribed to help keep cholesterol within the American Diabetes Association’s recommendations.
- Aspirin: Aspirin is often recommended for patients with diabetes to help protect their hearts, which are more susceptible to heart disease.
Monitoring Blood Sugar
Monitoring your blood sugar levels lets you know how well the other parts of your diabetes treatment are working. It also makes it easier to keep your levels in a range that makes you feel good and reduce the risk of developing more serious complications down the road.
Depending on whatever your doctor prescribes you relating to the hormone that regulates glucose in your blood, you may have to monitor and record your blood sugar level at least four times a day.
This is due to the fact that blood sugar levels tend to fluctuate unpredictably throughout the day, even when following a strict eating and hormone administering schedule. Among other things, your levels can be affected by food, activity, illness, medications, stress, hormonal changes, and alcohol.
To be safe, the American Diabetes Association recommends testing blood sugar levels before meals and snacks, before bed, before exercising or driving, and any time you suspect you may have low blood sugar.
Modern methods of monitoring blood levels include continuous glucose monitoring (CGM) in which a monitor is attached to your body using a fine needle just under the skin that checks blood glucose level every few minutes. However, CGM is not yet considered to be as accurate as standard blood sugar monitoring, so checking your blood sugar levels manually is still recommended.
Eating Healthy and Monitoring Carbohydrates
Since carbohydrates are converted to sugar (glucose) shortly after you ingest them, they (some more than others) cause your blood sugar levels to rise. As someone suffering from diabetes, you then need to take the hormone that regulates glucose in your blood to bring these levels back down. If the carbohydrate-to-hormone ratio is off, it can negatively affect your blood sugar levels, which can result in all sorts of complications.
No one diet is going to cure or treat your diabetes, but eating the right foods and counting your carbohydrates will make sure you always know how much of the hormone that regulates glucose in the blood is needed to properly metabolize the carbohydrates you’ve eaten.
The “right foods” in this case refer to nutritious, low-fat, high-fiber foods such as fruits, vegetables, and whole grains. Your doctor or dietician can recommend foods more specifically tailored to your age, activity level, schedule, and food preferences.
Exercising
Exercise is also an important part of diabetes treatment. In addition to medicine, exercise also helps keep blood sugar levels in a healthy range. It can also reduce the risk of other health problems, such as heart disease (something people with diabetes may be more likely to get).
Before starting to exercise, it’s important to consult with your doctor, especially if you suffer from complications like hypoglycemia (low blood sugar) or hyperglycemia (high blood sugar). These can flare up more often during physical activity.
It’s also important to constantly check your blood sugar levels as you exercise, especially if you’re beginning to exercise more often. You may need to adjust your meal plan or hormone doses to compensate for the increased activity.