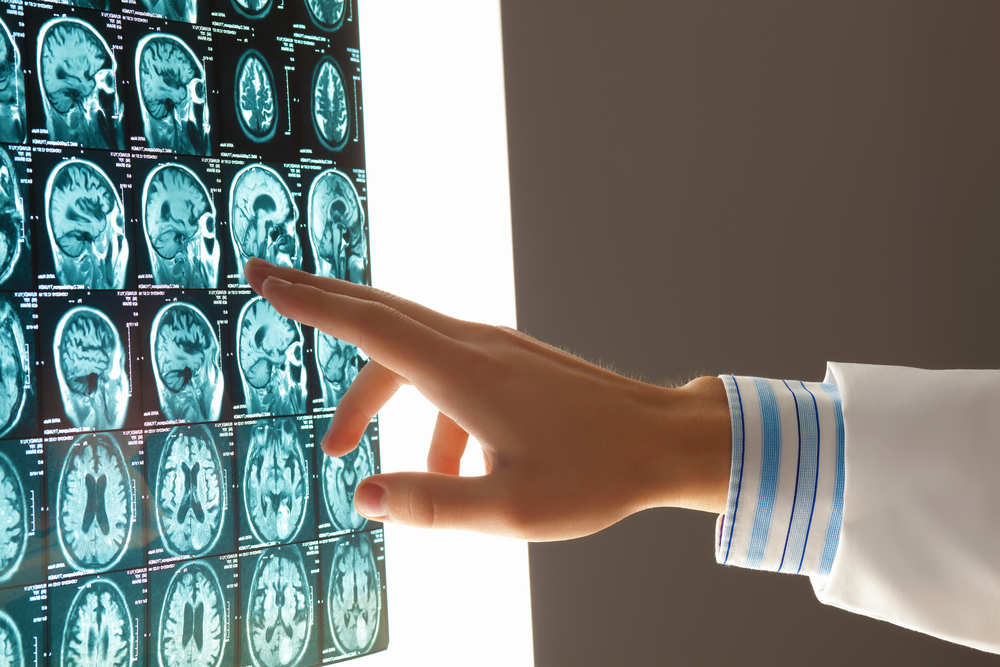
Traumatic brain injury (or TBI) occurs as the result of a traumatic event, which injures the brain. This can be a result of a penetrating injury or a closed injury. Brain damage can occur along the path where an object—such as a bullet or shrapnel—enters the brain. TBI can also occur as a result of sudden acceleration/deceleration of the structures of the brain within the cranium, for example if a hockey player receives a slap shot to the head or as the result of a fall.
TBI is a leading cause of death and disability. It is estimated that the annual incidence of mild TBI is 100 to 600 people per 100,000 worldwide. People between the ages of 15 and 24 experience the highest number of TBI’s. Males have twice the risk of sustaining a TBI than females and four fold the chance of resultant death. The next highest risks for TBI are children 5- to 9-years of age and adults over the age of 80. Let’s take a closer look at TBI and its symptoms…
1. Not All Symptoms Appear Immediately
A closed head injury can be misleading. Often the person is awake, talking and oriented immediately after sustaining a hit to the head. This can be the case after a motor vehicle accident, fall, or sports injury. The absence of any external injury coupled with seemingly normal cognition may give the false impression that everything is okay.
A severe, sudden hit to the head causes the brain to ricochet off the inside of the skull. Back and forth. This can produce internal bleeding and bruising which may continue long after the initial injury. This why a person must be monitored hourly for the first 24-hours after sustaining a concussion for any change in their level of consciousness. Should they become confused, lethargic or non-responsive, medical care must be sought immediately.
2. With Brain Injury 1+1 Does Not Equal 2
If you already have a pre-existing brain injury and receive another blow to the head (even years later), the effects are not that of 2 blows, but closer to 20 blows. One brain injury plus another brain injury can equal the effects of 20 brain injuries at once. This is because your brain is already damaged and vulnerable. This phenomenon is called the “thin skull” theory by personal injury lawyers. The medical term is delirium, which if left untreated can prove fatal.
Another life threatening condition known as second impact syndrome can occur spontaneously if a person sustains a second concussion before the first one is healed. In this instance the brain is unable to auto regulate and swells rapidly. Loss of consciousness, brain herniation, and death may occur. This syndrome is more common in athletes, such as football players, who are sent back into play after a hit to the head and sustain a second concussion.
3. Multiple Concussions Can Cause Long-Term Disability
In the past decade it has come to light that multiple concussions can cause permanent brain damage known as chronic traumatic encephalopathy (or CTE). One study of deceased NFL players found that upon autopsy, 76 out of 79 player’s brains showed evidence of severe CTE. Further studies on the brains of deceased college football players discovered small amounts of CTE in players as young as 18. CTE occurs when repeated hits to the brain cause the development of an abnormal protein called “tau”.
Players suffering with a mild to moderate CTE often develop depression, anxiety, poor judgement, alcohol or drug dependence and bouts of uncontrollable rage. More severe CTE suffers may experience confusion, memory loss, breakdown of social relationships, and dementia.
4. Brain Damage Can Cause Pseudobulbar Affect
This disturbing condition can be a source of distress and embarrassment for patients and family alike. Pseudobulbar affect (PBA) involves uncontrollable outbursts of crying or laughing in people with certain types of brain injury. PBA outbursts can be inappropriate for the situation and don’t always reflect how the brain injured person is actually feeling. This can be a source of embarrassment especially in social or family gatherings.
PBA outbursts can also be exaggerated. They may be expressed appropriately, but be overly intense. Or the brain injured person may experience difficulty turning off their emotions and cry or laugh for extended periods.
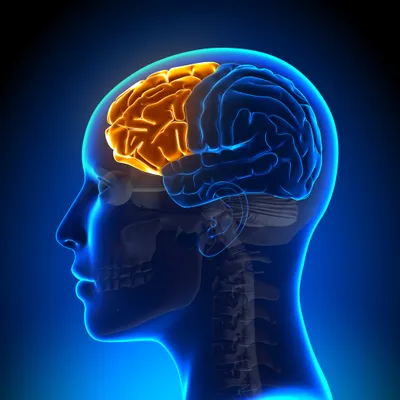
5. Frontal Lobe Damage
Damage to the frontal lobes can have devastating consequences for both individuals and their families. This area of the brain is responsible for higher level executive functioning—such as mood regulation, social behavior, decision making, planning, and problem solving. Frontal lobe syndrome otherwise known as dysexecutive syndrome consists of a cluster of common symptoms. People with frontal lobe damage typically have cognitive, emotional, or behavioral problems. On occasion they exhibit difficulties in all 3 areas.
People with frontal lobe damage are often prone to episodes of unprovoked explosive rage or aggression. Research conducted by Dr. Dorothy Otnow Lewis, a psychiatrist at New York University, and Dr. Jonathan H. Pincus, the chief of neurology at the Veterans Administration Hospital in Washington, found that every one of the death row convicts in their study had suffered a severe traumatic brain injury as a child prior to committing violent criminal offenses themselves.