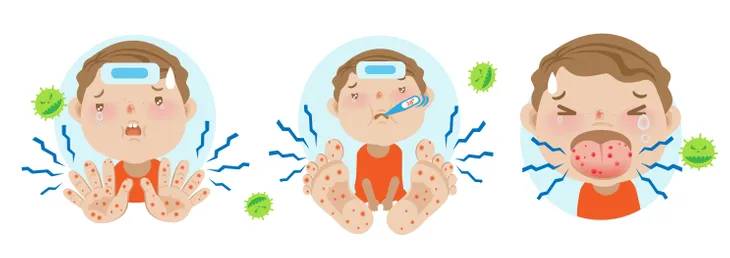
While hand, foot, and mouth disease is considered mild, at least by the Mayo Clinic, it doesn’t mean it’s pleasant. This contagious condition is common in children (especially when they’re regularly in a social setting such as a daycare) and is most commonly caused by the coxsackie virus.
The Mayo Clinic says symptoms can vary depending on the stage of the disease, but it usually doesn’t last very long (usually about a week). In some rarer cases, symptoms can become more severe, so keep an eye on them. The disease is more common in the fall.
Here’s everything to know about hand, foot, and mouth disease, including the signs, symptoms, and treatments…
1. Fever First
The Mayo Clinic says that the first sign of hand, foot and mouth disease is often a fever, followed by other symptoms such as a sore throat, and a loss of appetite, or generally not feeling well (known clinically as malaise).
The clinic notes that the other symptoms will usually show up 1 or 2-days after the fever starts, and the fever will generally last a few days. Of course, a fever can be tied to many other illnesses, so consult a doctor if symptoms don’t improve.
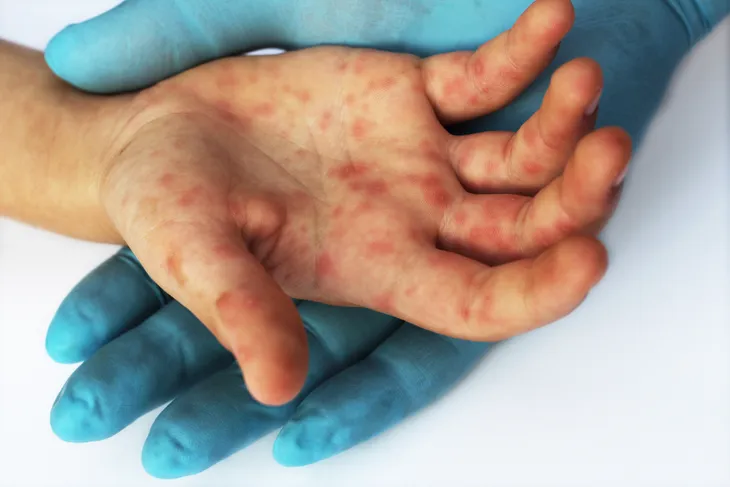
2. Rash Follows
As the name of the disease suggests, a rash can appear not only on the hands and feet but also on the buttocks, notes WebMD. “And while it’s not pleasant, it also isn’t serious,” assures the source.
WebMD notes that your child may get a rash on the palms of the hands or soles of the feet 1 or 2-days after the first symptoms appear (which, as we’ve already mentioned, will probably be a fever). The rash may worsen and turn into blisters, and you might notice sores on the knees and elbows.
3. Mouth Sores
KidsHealth.org talks about the other part of the illnesses namesake, noting “painful red blisters” can appear in the mouth and throat. In some cases, kids will have no skin signs of the disease other than sores in the back of the throat.
There could be other symptoms related to having pain in the mouth and throat. For example, the source explains your child may drool (due to painful swallowing) and may become more partial to only cold fluids.
4. Ulcers Only
The Women’s and Children’s Health Network (government of South Australia) reminds us that hand, foot, and mouth disease is primarily a children’s disease. This is because “most adults will have had the infection in childhood” and will likely not experience it again later in life.
However, if the virus does reappear in adults, it’s usually contained to ulcers in the mouth rather than the rash on the hands and feet.
5. More Severe Symptoms
The Seattle Children’s Hospital confirms there is a more severe version of the disease that became more prominent around the world in 2012 as a result of a “new” coxsackie A6 virus.
In this case, the rash, “made up of many small blisters,” can spread onto the arms, legs and face it. Skin peeling may occur. “It looks bad but is harmless,” adds the source, noting a skin moisturizer on the raw areas can help. Fingernails and toenails can fall off in some cases, but only in about 4-percent of the severe cases.
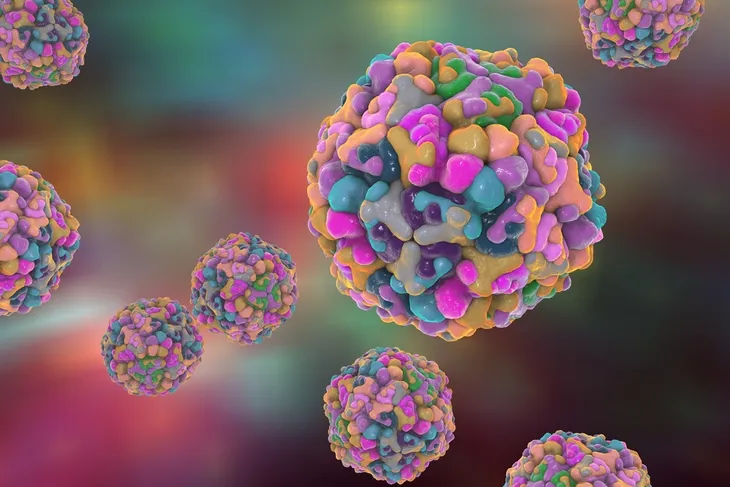
6. What Causes It?
As we previously mentioned, hand, foot and mouth disease is caused by the coxsackievirus. This particular virus is apart of a larger group of viruses known as non-polio enteroviruses, but the Mayo Clinic states that other enteroviruses can also sometimes cause hand, foot and mouth disease. According to the Montreal Children’s Hospital, the enterovirus family contains over 90 different types of viruses, many of which are responsible for frequent illnesses in children and infants.
A person will often contract the virus orally through person-to-person contact with another infected individual, says the Mayo Clinic. Some of the most common ways of it spreading are through nasal secretions or throat discharge, saliva, fluid from blisters, stool, or respiratory droplets in the air from a cough or sneeze.
7. Who is at Risk?
The people who have the highest risk are children under the age of 10, but more often it occurs in children who are under the age of 5. It’s also most commonly found in child care settings “because of frequent diaper changes and potty training, and because little children often put their hands in their mouths,” says the Mayo Clinic.
Children tend to develop immunity as they get older when their body builds antibodies after they’ve been exposed to the virus that causes the disease. But the Mayo Clinic does warn that it is possible for adults to get this disease.
8. How Long Does it Last?
While the infected person is most contagious in the first week of the illness, it can remain in the body for several weeks. You’ll likely know when it’s gone, as the signs and symptoms will disappear, but until they are gone for sure, the child (or adult) could still be contagious.
The Montreal Children’s Hospital states that the typical incubation period for hand, foot, and mouth disease is about 3 to 6-days, but the virus can still be present in stools for up to 8 to 12-weeks after the infection.
The Mayo Clinic warns that some adults, and even children, can spread the virus without showing any symptoms. Outbreaks of hand, foot, and mouth disease are most common in the United States during temperate months such as the autumn or summer season, but in more tropical locations, it can occur year-round.
9. How is it Diagnosed?
The diagnosis for hand, foot, and mouth disease is fairly simple. A doctor can make a diagnosis after performing a simple physical exam checking the mouth and body for the appearance of any blisters or a rash, says Healthline. They will likely also ask about some of the other symptoms listed in this article.
The doctor might require a throat swab or stool sample in order to test for the virus, which will offer a more conclusive diagnosis.
10. Limited Treatments
The Centers for Disease Control and Prevention (CDC) explains there is no specific treatment for this illness, although you can help relieve your child’s symptoms. It suggests over-the-counter pain relievers (but reminds that aspirin should not be given to children). You can also seek medical attention and receive some prescribed medications, but most are available without a visit to the doctor. Healthline lists some of these treatments as “prescription or over-the-counter topical ointments to soothe blisters and rashes, pain medication, such as acetaminophen or ibuprofen, to relieve headaches,” and “medicated syrup or lozenges to ease painful sore throats.”
You can also use mouthwash or sprays (or even chew on ice chips) to help numb the mouth and throat region your child is in a lot of pain. If these non-prescription methods don’t provide any relief, then you should contact your healthcare provider. Also make sure your child stays hydrated.
More often than not, hand, foot, and mouth disease should go away on its own within 7 to 10-days.
11. At-Home Treatments
Even though hand, foot and mouth disease can be a little scary for parents, it’s considered to be a minor illness that typically only lasts 7 to 10-days. You can contact a doctor and have them prescribe any of the treatments we listed above, especially if mouth sores or a sore throat are affecting whether your child can drink fluids or if symptoms seem to get worse instead of better, but it can also be treated with some simple at-home remedies.
Healthline lists simple remedies such as ice or popsicles, ice cream, or cold beverages. The source also recommends avoiding citrus fruits, fruit drinks, soda, and spicy or salty foods.
12. Preventative Measures
Of course, as with any disease, the best way to beat hand, foot, and mouth disease is to avoid getting it in the first place (which is easier said than done). You can avoid catching the disease by not touching the blisters or stool of a child that you know to be infected, explains MedicinePlus.gov.
To help prevent your little one from passing the disease along to their friends, you should keep them home from daycare until the fever is gone (usually around 2 or 3-days). However, if there’s many blisters still visible, you should avoid letting your child go to school or daycare until they dry up, usually around 7-days, according to the Seattle Children’s Hospital.