Considered by the March of Dimes as the most prevalent types of birth defects, congenital heart defects (CHDs) are considered deadly health conditions that a baby is born with.
CHDs change the function and/or shape of a newborn’s heart (or parts within) to the point that overall health is compromised, which means treatment is typically required within the first hours, days, or months of life. Here are 7 important facts to know!
1. CHD Statistics
The website, LittleHearts.org, estimates that 40,000 U.S. babies are born with CHD annually each year—that’s roughly 1 in every 100 newborn (or 40,000 babies).
In many cases heart defects don’t require treatment or are easily fixed. However, in serious cases or babies born with critical congenital heart disease (or CCHD), the heart defect can result in deadly health issues and requires immediate attention.
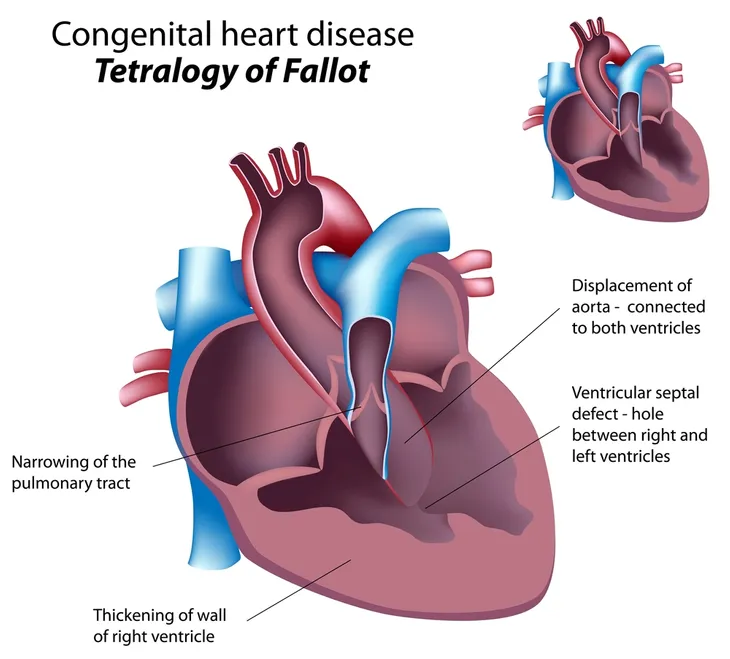
2. How Heart Defects Affect the Heart
Heart defects can develop and cause issues in many parts of your baby’s heart. For instance, heart defects can the blood flow in the heart via the arteries and veins (blood flow from the body to the heart).
Alternatively, heart defects can impact the heart via the heart valves (which control flow to and from the heart) or via the septum (which divides the heart’s left and right sides).
3. Causes of Congenital Heart Defects
Medical researchers know that CHDs develop when the heart is still forming, during very early pregnancy. Although they’re uncertain of a direct cause, medical experts deem several factors can be at play in CHD development. For instance, there is a link between CDHs and expecting mothers who contract rubella (or german measles) or are considered obese (a BMI over 30).
Expecting moms with lupus (an autoimmune disease that impacts heartbeat), some cases of phenylketonuria (or PKU, which blocks the breakdown of the amino acid phenylalanine), and diabetes (due to blood glucose) are also prone to delivering babies with CDHs.
4. Chromosomal and Genetic Conditions
Babies are also prone to heart defects if certain gene or chromosomal mutations are present. For instance, Stanford Children’s Health estimates that 30-percent of babies with a heart defect also suffer from a genetic or chromosomal condition—such as noonan syndrome, down syndrome, alagille syndrome, velocardiofacial syndrome, and turner syndrome.
The presence of a congenital heart defect in a parent may also increase the risk of your your baby being born with a CHD.
5. Lifestyle Factors
Research from the University of Maryland Medical Center also considers CHDs in babies dependant on certain lifestyle factors. For instance, if pregnant women take certain medications taken for health issues (i.e., to treat bipolar disorder, acne, or seizures) the incidence of CHD can increase in their babies.
In addition, smoking and drinking alcohol while pregnant have also been shown to increase the risk of delivering a baby with a CHD.
6. Diagnosing CHDs During Pregnancy
Many serious CHDs are diagnosed during pregnancy or very shortly after delivery using standard tests. For instance, fetal echo tests are often used to monitor and capture a picture of your unborn baby’s heart, between the 18- and 22-week of pregnancy.
Your doctor will typically recommend a fetal echo test if mom has an existing medical condition (i.e., a CHD, diabetes, or lupus). Your doctor may also recommend the test if either parent has a family history of heart disease or CHDs, if your baby’s heartbeat shows up as abnormal during an ultrasound, or if your baby has a chromosomal condition (i.e., turner or down syndrome).
7. CHD’s in Older Children
Often, if the CHD is not as severe heart defects, it may not be diagnosed until after delivery via a newborn screening—when hearing, heart, blood, and oxygen in blood (or pulse oximetry) tests are performed at the hospital.
In the hours and days after baby is delivered, hospital staff check and monitor the baby for signs of heart defect. If they notice an abnormal heart murmur, breathing difficulties (too fast or labored), perspiration while feeding, fatigue, changes in skin color, slow weight gain, and swelling (in the belly, legs or eye area), a CHD may be present. If your baby shows any of the above symptoms after leaving the hospital, seek immediate medical attention.