A stroke is always just a stroke, right? Not always. There are the classic strokes that cause all the telltale signs, such as slurred speech and numbness in the limbs on one side, and then there are something called mini-strokes (also known as transient ischemic attacks or TIAs), which should also be taken seriously, despite the name.
There are many similarities in the symptoms of a mini-stroke and a full-blown (ischemic) stroke, but the outcomes are different. A mini-stroke may also serve as a warning that a bigger health episode is on its way. Let’s take a closer look at 12 differences and similarities between them…
Defining a TIA
A mini-stroke can be defined as an episode of brief blockage of blood flow to the brain, which does not result in permanent brain damage, explains Self.com.
In the case of TIA, the blockage will break up and clear on its own, without medical intervention. However, as we’ll get to soon, you’ll see that it will be hard to distinguish which type of stroke a person is suffering from so they should all be taken seriously.
Explaining an Ischemic Stroke
Unfortunately, most strokes fall into this more serious category, which can be broken down into two subtypes (thrombotic and embolic), explains WebMD. An ischemic stroke is caused by a fatty buildup (also called plaque) in your arteries and narrows them, subsequently impeding the flow of blood.
A thrombotic stroke is the result of a blood clot in an artery that feeds the brain, while an embolic stroke forms elsewhere in your body and then travels to your brain, adds the source. These types of strokes will cause brain damage, but the extent will differ by case.
Diagnosing the Type
It can be tricky in some cases to determine which type of stroke a patient has suffered, especially in the case of a mini-stroke, because the symptoms will disappear by the time the victim is evaluated.
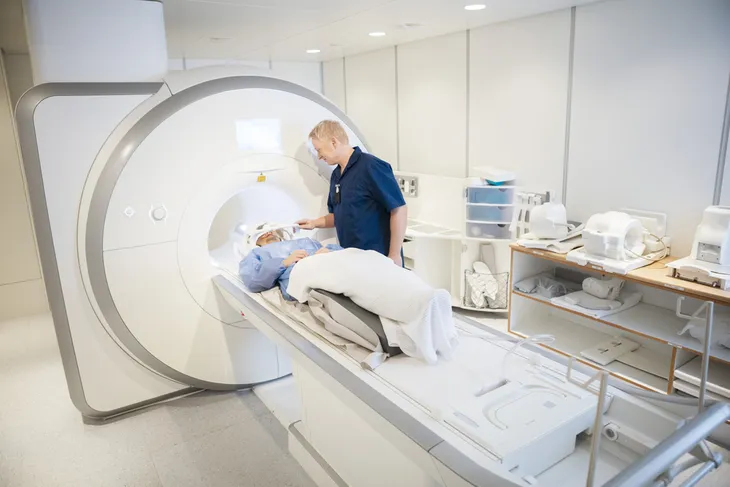
Healthline.com explains the only way a doctor can tell the difference between a TIA and an ischemic stroke is by using a scan (CT or MRI) to pinpoint damage. However, it may take up to 48-hours for any signs to show up on a CT scan, while MRIs usually present evidence sooner, adds the source.
They’re Hard to Distinguish by Symptoms
A mini-stroke will present with all the symptoms of a classic stroke, although it lasts for a shorter period of time, notes MedicineNet.com. These telltale symptoms include weakness or numbness in the arm or leg on one side of the body, as well as dysphasia (trouble speaking).
Other similar symptoms include dizziness, sudden changes in vision, tingling sensations, confusion, loss of balance, and passing out. “Symptoms of a stroke include those of a mini-stroke, but the symptoms do not resolve,” notes the source.
Lingering Symptoms of Stroke
While the problems associated with a mini-stroke will often disappear completely within 24-hours, there can be certain long-term effects from a stroke that can make life more challenging for a victim.
For example, many stroke patients experience dysphagia, which is the medical term for trouble swallowing, according to the National Stroke Association. While someone experiencing TIA can have temporary speech problems, a full stroke can result in dysphasia, which is longer-term difficulty with communication as a result of brain damage.
It’s All About Timing
Healthline explains that the symptoms of a stroke can last more than 24-hours, while a mini-stroke can last anywhere from a few minutes to a few hours (but less than 24-hours). Because mini-strokes don’t persist, “many people make the mistake of not seeking medical treatment since the symptoms are less severe,” says the source.
In the case of an ischemic stroke, there will almost always be permanent damage that will take a considerable amount of time to recover from through rehabilitation. However, with a mini-stroke, quite often the patient will carry on as if nothing happened.
One Thing Leads to Another
You may think you got away with just having a mini-stroke, but the National Stroke Association says this is often a red flag that something more serious could be on its way. “While TIAs generally do not cause permanent brain damage, they are a serious warning sign that a stroke may happen in the future and should not be ignored,” it adds.
The source also has a TIA risk calculator to help you determine how much of a stroke risk you are, but keep in mind sources say you should always follow up with a doctor following a mini-stroke for an assessment and possible preventative treatments.
Treatment for TIA
The Mayo Clinic explains once a doctor has determined you’ve suffered a TIA, then a regimen of medications to improve blood flow to the brain can be given (or current prescriptions adjusted).
These drugs can include over-the-counter aspirin, antiplatelets, and anticoagulants. Doctors may even suggest surgical procedures to open up clogged arteries. “It also requires identifying abnormalities that your doctor can fix to reduce your risk of future TIAs or strokes,” says the clinic.
Treatments for Ischemic Stroke
The American Heart Association says getting immediate treatment for a stroke is key to limiting the damage. In the case of ischemic stroke, the lone FDA-approved treatment is tissue plasminogen activator (tPA, also known as intravenous [IV] rtPA, which is given through an IV in the arm). It works by dissolving the blood clot and restoring blood flow to the brain, adds the source.
Aside from that option, medical professionals can also resort to a mechanical thrombectomy, which involves threading a catheter through an artery in the groin to the site of the blockage in the brain, it explains.
Recovering from a TIA
In the case of a TIA, all of the symptoms often disappear within 24-hours with no sustained damage, notes the Better Health Channel in Australia. That means the patient will have a full recovery in most cases, but it doesn’t mean they’re in the clear.
A TIA “provides a powerful warning that a stroke may follow in the next few hours, days, weeks or months,” adds the source. Following prescriptions and making lifestyle changes, such as quitting cigarettes, lowering fat in your diet, and exercising regularly can help reduce the risk of a full stroke.
Recovering from a Stroke
The area of the brain affected by a stroke can determine recovery outlook, notes the American Heart Association. “The most rapid recovery usually occurs during the first three to four months after a stroke,” but the patient can continue to improve after that, adds the source.
The patient’s desire to recover and his/her prior health, as well as having quality caregiver support, will determine how long it takes to get better following an ischemic stroke, says the source. It warns that post-stroke depression is common and can hinder the recovery process.
Shared Risk Factors
The Mayo Clinic says the risk factors for TIA and stroke are similar. There are some risk factors you can’t control, while other risk factors you can control. For example, family history, age (55-and older), and gender (slightly more common in men) are all things you can’t do anything about.
However, other risk factors, such as high blood pressure, high cholesterol, smoking, excess weight, and poor nutrition, are all avoidable, although you may want to enlist the help of a medical professional to get on the right track.