Perimenopause is referred to as the final cessation of your menstrual cycle and the time in which you will start to see and feel the signs and symptoms of menopause, including weight gain, hot flashes, and mood swings. Perimenopause differs for every woman, but on average, it takes about a year to complete (unless you have a full hysterectomy) and occurs between the ages of 45 to 55, after which time you are postmenopausal.
Here are 20 common signs and symptoms that you are perimenopausal…
Experiencing menopause symptoms? Try DrFormulas Menopause Supplements – an Amazon 4.5+ star bestseller with over 1,500 consumer reviews. (As an Amazon associate, this site earns from qualifying purchases).
Missed Periods
Your “time of the month” is typically regular, but when your period doesn’t show up on time, gets shorter and lighter, or you start to clot heavily, it may signal menopause is approaching. Odds are, if you’re getting up there in age (or aren’t sexually active), your missed period is not from pregnancy but instead is a sign that you may be starting menopause.
During the menopausal transition period, your cycle may never be what you normally experience. And the first time you notice these changes, you might feel emotional or upset, both from changes in your hormone levels and the significance of this lifetime milestone. Although the average age of menopause is 51, some women go through it much earlier — some are younger than 40 — or much later, so when your period changes at any time, you should see your doctor. Remember, full menopause occurs when you’ve gone a full 12-month period without menstruation.
Hot Flashes
Just about any woman approaching menopause knows a hot flash when she feels one. That sudden overwhelming blast of heat that extends from your forehead to your toes and leaves you soaking with sweat occurs due to hormones mixing up your body’s temperature regulation (the hypothalamus). You can experience hot flashes all over your body or in just one area, but the extreme temperature change in your body is uncomfortable no matter where you feel it.
Your face may also flush and turn red or become blotchy, and the severity of your hot flashes can range from mild to quite severe – some women are woken up from sleep because of them, causing additional fatigue. There are some treatments available for hot flashes but many of them come with side effects. Knowing your options is important, so make sure your doctor is aware of your symptoms. Unfortunately, hot flashes can last for a couple of years after menopause.
Weight Gain
Weight gain can be a very frustrating attribute of menopause, especially since the added weight tends to accumulate in the midsection, one of the worst areas to gain weight. So as you age, it’s important to maintain a healthy lifestyle because studies have shown that postmenopausal women are at increased risk of heart disease – weight gain around your midsection is linked to heart disease, on top of the fact that extra padding in your belly is very difficult to get rid of.
You could also gain weight by changes in your diet (eating unhealthy foods) and from a lack of exercise. Try to combat weight gain by consuming a healthy diet rich in nutrients and enjoying some regular exercise. It’s a good time to try out a new exercise class with friends or spend time with family doing something active. Exercising can help with more than just your physical health – exercise could help you mentally and emotionally deal with other symptoms and changes associated with menopause.
Sleep Deprivation
Insomnia is typical to women in perimenopause, as estrogen levels deplete and the brain excretes fight-or-flight response chemicals that keep you on high alert through the night. You may have difficulty falling asleep, as well as staying asleep. Sometimes hot flashes contribute to sleep deprivation, because when they’re severe, they can wake you up and keep you awake several times throughout the night.
Many women find that regular exercise accompanied by melatonin supplements helps them get their blissful sleep back. Another good way to help you sleep is to do breathing exercises. They can help calm you down, especially when being unable to sleep causes your mind to race or anxiety to build. Breathing through your nose, inhale slowly for four seconds and exhale slowly for four seconds. Do several repetitions. Meditation is another technique that’s been known to help relax your body and mind, which could help you fall asleep. And who knows, you might find a technique that’s so beneficial to your overall health that you continue doing it when you’re postmenopausal.
Vaginal Dryness
An unfortunate and uncomfortable early warning sign of menopause is vaginal dryness. As estrogen decreases so does the body’s lubrication and moisture in the skin, hair, and more intimate areas such as in the vagina, which can make sex suddenly painful or uncomfortable. Talk to your gynecologist about over the counter lubricants to help increase moisture and sexual enjoyment. It’s best to address the vaginal dryness head on – sex should never be painful and there are options available to make sure it never is.
Some of your options to get rid of dryness include gels, prescription oral and cream medications, and vaginal rings. Hormone replacement therapy (HRT) is another option. HRT gets your body to produce its natural lubrication, but it must be prescribed to you by your doctor. There are also some easy changes you can make to your body washing routine to help with vaginal dryness – stop using soap to clean your vagina or try a soap-free cleanser.
Mood Swings
PMS like pregnancy and menopause leaves the hormones unbalanced, often resulting in outbursts of anger, irritability, or crying for no reason. It can seem like your mood changes from one second to the next, and your inability to control it can be frustrating, confusing and upsetting. If you add to that sleep deprivation, and the fear and confusion over the changes taking place in your body, it’s no wonder you’re a bit cranky.
It might not seem like much consolation, but going through menopause is a transition in life women around the world experience – you’re not alone! Try focusing on the good things in your life, sign up for a new community class (like a hobby or exercise course) and take some control back by adding relaxation techniques to your daily ritual. Learning things that can calm you, such as yoga or breathing exercises, can help you deal with mood swings when they happen and lessen the negativity you feel afterwards.
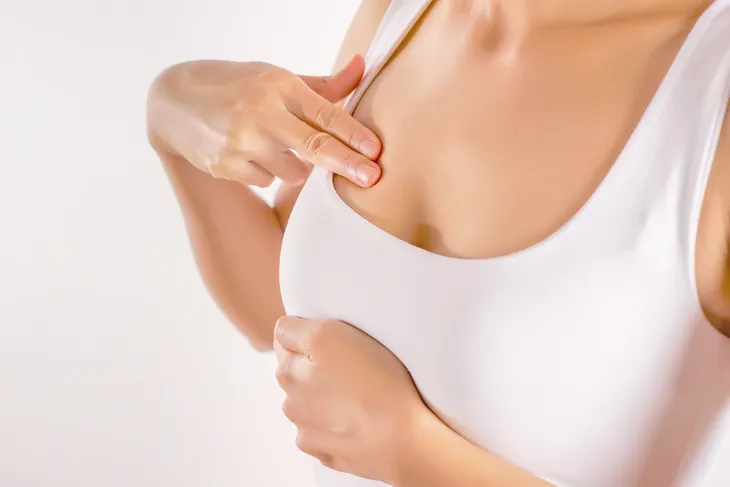
Sore Breasts
Sore, tender breasts are often a sign of menstruation, pregnancy, and menopause due to hormonal changes, water retention, and swollen breast tissues. In the meantime, you may want to buy a comfortable bra with added support and cut out excess caffeine, which can aggravate swelling and water retention. For some women, they also experience swollen breasts to go along with the tenderness. Sometimes hormone medication and creams – specifically progesterone to balance the spike in estrogen during perimenopause – can help relieve and prevent these symptoms.
Even if you are still getting your period once in a while, breast tenderness isn’t limited to before your cycle. Unfortunately, it could happen at any time. The severity in which you experience this pain can range from mildly uncomfortable to really painful, even with just the lightest touch. Discuss your options with your doctor if breast tenderness is causing a lot of discomfort. Your doctor could recommend an over the counter medicine or decide to prescribe one.
Chronic Headaches
As certain hormones deplete, certain foods (i.e., caffeine) can aggravate neurological changes in our brains. Migraines are often a painful symptom of perimenopause, and excess coffee, noise, and bright lights never help those who suffer from chronic headaches. While hormone levels fluctuate during the early stages of menopause, the intensity of headaches and migraines can worsen. Added stress, which can easily be a result of other perimenopausal symptoms such as insomnia and mood swings, can increase the risk of migraines during these early stages.
Women who are prone to headaches or migraines from hormonal changes, such as around and during their period, are at a higher risk to experience them during perimenopause. Hormonal headaches are due to a decrease in hormones that stimulates the headache. Menstrual headaches are due to the decrease in estrogen and progesterone at that time of the month. Generally, women on HRT do not have more headaches, but instead actually improve.
Decreased Sex Drive
As women transition into menopause, they often feel one of two extremes. While some feel sexually liberated now that they are no longer able to get pregnant, others suffer sudden self-consciousness and feel undesirable. Hormonal changes can contribute to feelings of depression and self-consciousness, and you could experience lack of interest in engaging in any form of physical intimacy. Many times testosterone hormone therapy can help restore some of that lost libido. Remember that although you can no longer get pregnant after menopause, you’re still at risk of contracting sexually transmitted infections or HIV, so while it’s good to feel sexually liberated, there are still risks.
Experiencing vaginal dryness and tender breasts can also impact your sexual desires. The idea of pain from touching and the actual act of intercourse can send you running in the opposite direction. But there are treatments and medications that can reduce these symptoms, and learning about your options from your doctor could help bring back some of your sex drive.
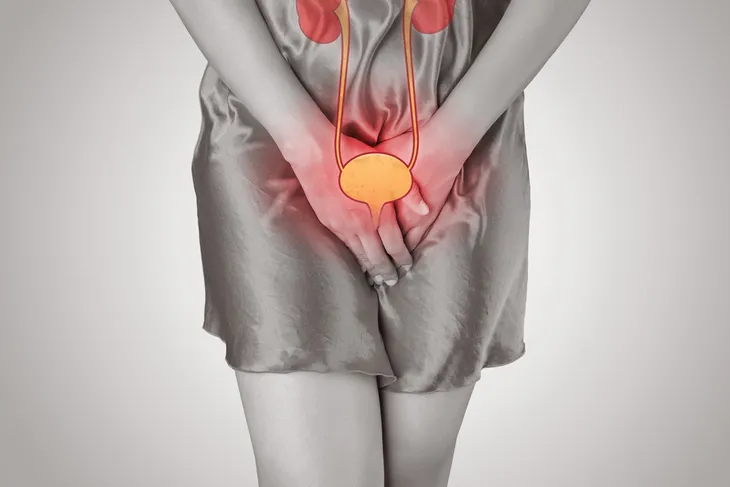
Incontinence
Do you suffer an embarrassing leak when you sneeze or jump up and down? Do you find it hard to get to the bathroom in time or does the need to urinate come on quickly? Bladder changes are typical during perimenopause as estrogen decreases and leaves the pelvic and bladder muscles weaker than normal. You can try Kegel exercises to strengthen the muscles of the bladder and pelvic floor.
If you’re really struggling with incontinence, there are adult disposable underwear, liners and pads that can prevent leaks from showing through your clothing. Although leaks are a common symptom of perimenopause and aging, it can be quite embarrassing and stressful if you’re prone to leaks. Nowadays, there are so many options for these products – many of which can’t be noticed or seen through your clothing. So get your comfort back and use incontinence disposable products if it happens regularly. And don’t forget to keep your doctor informed about any perimenopause symptoms.
Night Sweats
In addition to having hot flashes, many women who are approaching menopause also experience night sweats. With night sweats, you may wake up from sleep with a racing heart rate, your skin feeling cold and clammy, and your bed soaked in sweat.
Like hot flashes, night sweats are caused by changes in estrogen levels. These hormonal fluctuations confuse the hypothalamus (the region of the brain that controls body temperature) into thinking you have an elevated body temperature, which it attempts to remedy by triggering the sweat glands.
Memory Problems
If you suddenly find yourself being more forgetful than normal, or feeling like you’re in a constant state of brain fog, it may be an indication that you’re starting menopause. Once again, hormones are to blame for this.
As progesterone levels decrease due to missed periods, the body’s excess estrogen turns into a stress hormone, which impacts the part of the brain responsible for memory. If your memory problems are interfering with your day-to-day life, be sure to speak to your doctor as they may recommend HRT as a short-term remedy.
Chronic Urinary Tract Infections
Urinary incontinence isn’t the only type of bladder issue that can affect women in perimenopause; they may also experience urinary tract infections (UTIs). With a UTI, you may feel the need to urinate much more frequently, and when you do, the urine may be dark or bloody and cause you to feel pain or a burning sensation.
But why do they occur with perimenopause? As with the other signs mentioned on this list, hormone changes are the culprit. These changes can cause vaginal bacteria to change as well along with the tissue thinning or becoming atrophic, which increases your risk of not only getting a bladder infection but also experiencing them on a chronic basis.
Changes to Skin and Hair
It’s natural to experience changes in your skin and hair as you age. “Loss of fatty tissue and collagen will make your skin drier and thinner, and will affect the elasticity and lubrication of the skin near your vagina and urinary tract,” explains Healthline.
But getting closer to menopause may contribute to these changes as well. Lower levels of estrogen, for instance, may cause hair to feel brittle, dry, or even fall out. Skin may also be more prone to developing wrinkles, as well as acne blemishes and eczema flare-ups.
Increased Hair Growth
While you can lose hair during menopause, you can also grow hair on other parts of the body. Hirsutism is a condition that causes excessive hair growth in women on the upper lip, chest, back, abdomen, and other areas.
Hormonal changes of menopause may lead to women growing facial hair. These hairs can appear thicker, coarser, and darker than standard peach fuzz. So instead of finer hairs you may be used to, someone going through menopause may grow a more noticeable mustache and whisker hairs.
Anxiety or Depression
Your body goes through a lot of hormonal changes during menopause. In turn, the Cleveland Clinic says those changes can also affect chemicals in your brain. This means your mental health could be impacted with anxiety, depression, or even panic attacks.
While you may experience some anxiety or depression because of the changing hormone levels, frequent and ongoing symptoms of these mental illnesses are not the norm. You should seek help for your mental health if those feelings persist or grow more intense.
Decreased Muscle Mass
We know that menopause leads to a drop in estrogen levels. That decline impacts a number of bodily functions such as muscle mass. Estrogen works to increase visceral fat mass. When the body has less estrogen, this can lead to decreased bone mass density, muscle mass, and strength.
One study shows women will go through a decline of 0.6 percent per year of muscle mass after menopause, with other health and age-related factors also contributing to this statistic. The loss in muscle mass can lead to weakness and decreased mobility.
Slowed Metabolism
One major reason why people will gain weight during menopause is due to a slower metabolism. When you lose muscle mass, the rate at which your body uses calories slows down. This makes it easier to gain weight. Mayo Clinic says menopausal women are more likely to gain weight around the abdomen than the hips and thighs.
Some lifestyle changes you can implement to counteract your slower metabolism is by exercising more and eating a healthy diet. Preventing excessive weight gain will lower the risk of developing other health problems such as breathing issues, heart disease, and type 2 diabetes.
Dry Eyes
Even your eye health can be impacted by menopause. Dry eyes can occur because once you reach the age of 50, your tear production decreases. Healthline explains how tear production is what covers and lubricates the eyes. When your tear production declines, this can lead to a gritty, stinging, burning, or irritated feeling. Luckily, it’s one of the lesser known symptoms that not everyone will experience.
Increased Risk of Other Diseases
As mentioned earlier, menopausal women have an increased risk of developing heart disease. Not only is this due to the extra weight that is often put on in the body’s midsection during this time but also is a result of decreased estrogen levels.
Additionally, these hormone changes can cause women nearing menopause (and afterward) to experience loss of bone mass more rapidly than the body is able to replace it. This makes menopausal women in all stages more likely to have weak bones, experience fractures or breaks, and possibly even develop osteoporosis.
Experiencing menopause symptoms? Try DrFormulas Menopause Supplements – an Amazon 4.5+ star bestseller with over 1,500 consumer reviews. (As an Amazon associate, this site earns from qualifying purchases).