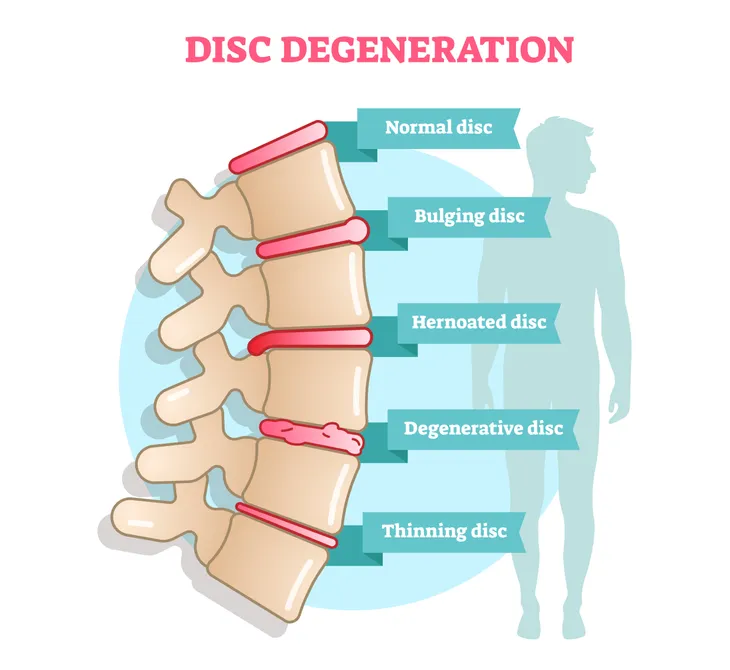
Our spinal discs, which are between our backbones, act as shock absorbers in the spine, giving us flexibility and allowing us to resist different forces of motion. Everyone’s spinal discs will experience some degree of wear and tear with age, but some people will actually develop degenerative disc disease, which is a condition that occurs when a damaged disc causes pain. It can lead to a wide variety of symptoms that vary in severity.
According to Cedars Sinai, the typical person with degenerative disc disease is active and in his or her 30s or 40s. They’ll also experience more pain and discomfort than the average person, particularly in their lower back (which may radiate down their leg). To get better informed on this topic, let’s take a look at the most common symptoms of degenerative disc disease, as well as the potential causes.
What is Degenerative Disc Disease?
Degenerative disc disease is an age-related disease that occurs when the normal wear and tear of our spinal discs starts to cause pain. Spinal discs are those rubbery discs that sit between the vertebrae (or bones) in the spine to absorb shock and allow us to stand up straight. They also keep us flexible, allowing us to move freely by bending and twisting. They also provide height.
Naturally, as we get older, they tend to break down or not work as well, says WebMD. For most people, the normal wear and tear of these discs doesn’t lead to any pain, but for people with degenerative disc disease, it will cause pain. We all get some form of back pain from time to time, but anyone with severe or chronic pain, particularly when sitting for long periods of time may have this condition.
What Causes It?
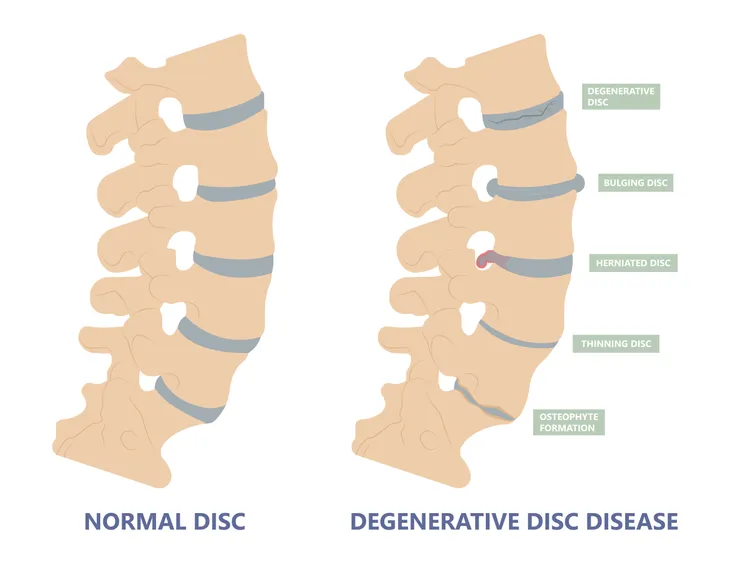
Our spinal discs are made up of a soft inner core and a tough outer wall. The following are changes that can occur to these discs, which could then result in degenerative disc disease.
Desiccation (or Drying Out)
When we are born, the discs in our spine are made up of water, says WebMD. As we get older, they lose water and get thinner. Over time, this water loss causes the discs to become flatter, which means they can’t absorb shock as well. It also means there is less cushioning or padding between each vertebrae. This is what leads to pain and problems in the spine, explain the source.
Cracking/Tearing
The other potential cause behind degenerative disc disease is cracking. The wear and tear of our everyday movements and potentially any injuries that we encounter along the way as we age can cause tiny tears in the outerwall of the disc, which contains nerves. These tears can become quite painful.
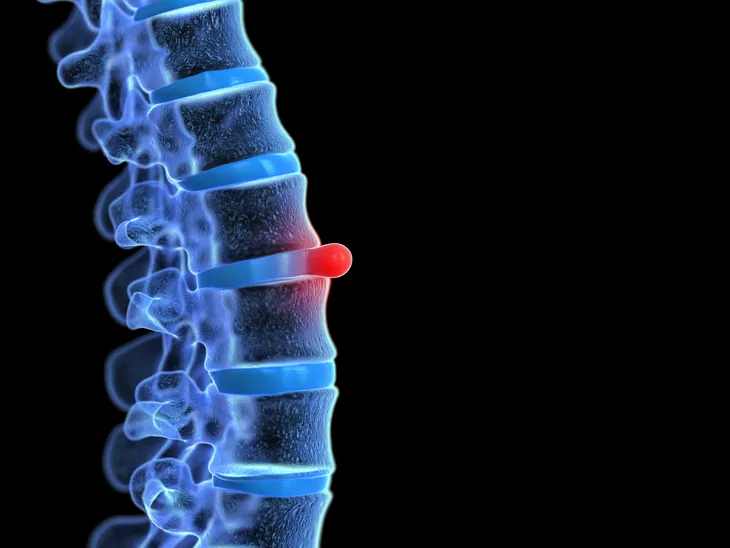
“If the wall breaks down, the disc’s softcore may push through the cracks. The disc may bulge, or slip out of place, which is called a slipped or herniated disc. It can affect nearby nerves,” writes WebMD.
Symptoms
Areas of Pain
Not surprisingly, one of the most common symptoms of degenerative disc disease is pain. The pain will be sharp and consistent, says WebMD. It can also be so debilitating that it interferes with daily activities. However, it’s important to note that some people can have this condition and not experience any pain at all. The severity of symptoms varies accordingly.
While it’s also obvious that this pain would be located in the back, it can occur in other areas of the body. Pain can occur in the lower back, buttocks, thighs, or the neck. The area of the pain depends on location of the affected disc. In some cases, it can also radiate into the arms and hands. It typically gets worse with age and may even lead to osteoarthritis, says Medical News Today.
Increased Pain When…
The pain that a person experiences with degenerative disc disease will be worse during certain activities, and may ease up at other times. For the most part, it all depends on the positioning of the body and how much pressure is on the spine. For example, pain will increase when sitting. “While seated, the discs of the lower back have three times more load on them than when standing,” says Cedars Sinai. Pain will also increase when bending, twisting, or lifting something heavy.
This pain is also increased when holding a certain position for an extended period of time. Spine-Health notes that this exacerbates low back pain. Other causes of problem might be looking down too long, as with a cell phone or book, which only worsens neck pain.
Decreased Pain When…
Just as the pain can increase during certain activities or positions, it can also decrease. For those who have degenerative disc disease, they may notice that their pain gets better when they are walking or even running compared to when they are sitting or standing. This again has to do with the weight and pressure on the back. It may also get better when changing positions or lying down.
You’ll likely want to change positions frequently to relieve the pain. Staying in one position for long periods of time can make the pain worse. You should regularly stretch the neck to decrease cervical disc pain. “[T]aking short, frequent walks during the day can decrease lumbar disc pain,” says Spine-Health.
The pain may also decrease when sitting in a reclined position or lying down with a pillow under the knees, adds the source. Another thing that could help is using a pillow to support the neck and its natural curve during sleep.
“Giving Out” Sensation
Spine-Health credits this “giving out” sensation to spinal instability. This instability is a result of the neck or back being unable to provide basic support. When this occurs, they will lock up and make any kind of movement difficult, similar to a muscle spasm (which we’ll talk about next).
Muscle Tension and Spasms
Another common effect of spinal instability is muscle tension and spasms. For some “lucky” people who have degenerative disc disease, they may experience no pain at all. However, these are the people who are more likely to have muscle spasms that are severely painful and can be temporarily debilitating, says Spine-Health.
According to Medical News Today, these muscle spasms are the body trying to stabilize the vertebrae which can be quite painful.
Radiating Pain
The pain associated with degenerative disc disease changes depending on the position of the body, but it can also come in waves of “radiating pain” that causes periods of intermittent severe pain. It may also feel like a sharp, stabbing or hot sensation. According to Spine-Health, pain flare-ups may be related to activity or abnormal stress on the spine, as well as occur with no reason at all.
“In cases of cervical disc degeneration, this pain is felt in the shoulder, arm, or hand (called a cervical radiculopathy),” writes Spine-Health. “In cases of lumbar disc degeneration, pain is felt in the hips, buttocks, or down the back of the leg (called lumbar radiculopathy).”
These periods of pain can last anywhere from a few days to a few months before they get better. It can also range from disabling pain to just a nagging pain that causes some discomfort. Eventually, the pain will return to at a low level or temporarily go away altogether.
Numbness and Tingling
A person can also experience numbness and tingling in their extremities, however according to WebMD, this only occurs in some cases. This numbness and tingling will occur in the arms and legs. According to the source, “It means the damaged discs may affect the nerves near your spine.”
Weakness
As we mentioned earlier, the symptoms of degenerative disc disease can occur in other areas of the body besides the back. One of these would be weakness in the leg muscles or foot drop. If this symptom is occurring, it’s likely a sign of damage to the nerve root, says Cedars Sinai.
Chronic Pain
Again, some people with degenerative disc disease will experience chronic pain, which is pain that is severe and totally disabling. “The amount of chronic pain — referred to as the baseline pain — is quite variable between individuals and can range from almost no pain or just a nagging level of irritation, to severe and disabling pain,” writes Spine-Health.
This type of pain can happen in people with degenerative disc disease, but it is extremely rare.