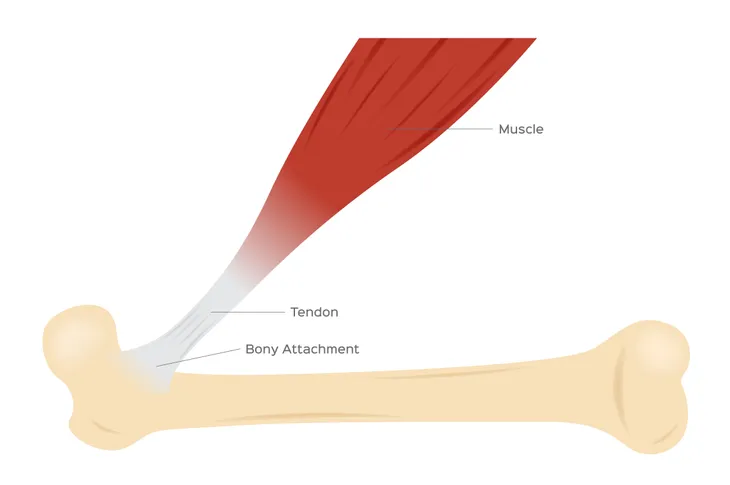
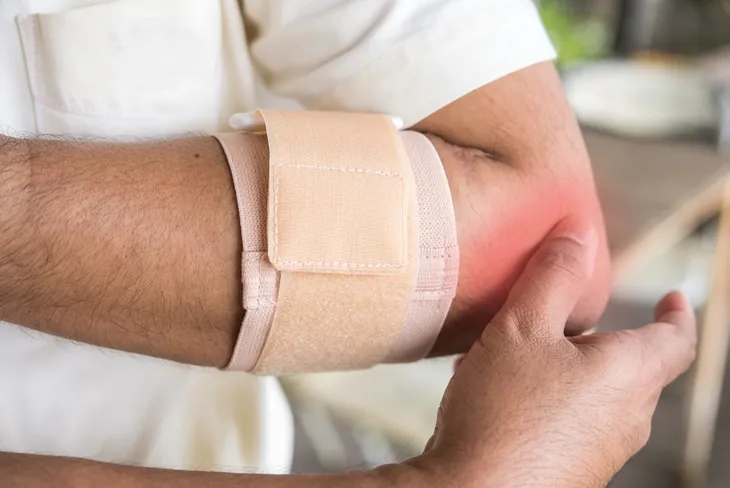
While your muscles and bones might be in great shape, you can still experience pain and limited motion. Why? You could have an inflamed tendon, which is a condition known as tendinitis. A tendon is a fibrous cord that connects a muscle to bone.
You might already know tendinitis by some of its nicknames, which refer to the places in the body where it commonly pops up. These include tennis elbow or jumper’s knee. However, tendinitis is not limited to certain places. The Mayo Clinic notes that it can happen in any tendon. Here’s what you need to know, including the signs, symptoms, and treatment options…
Repetitive Motion Is a Culprit
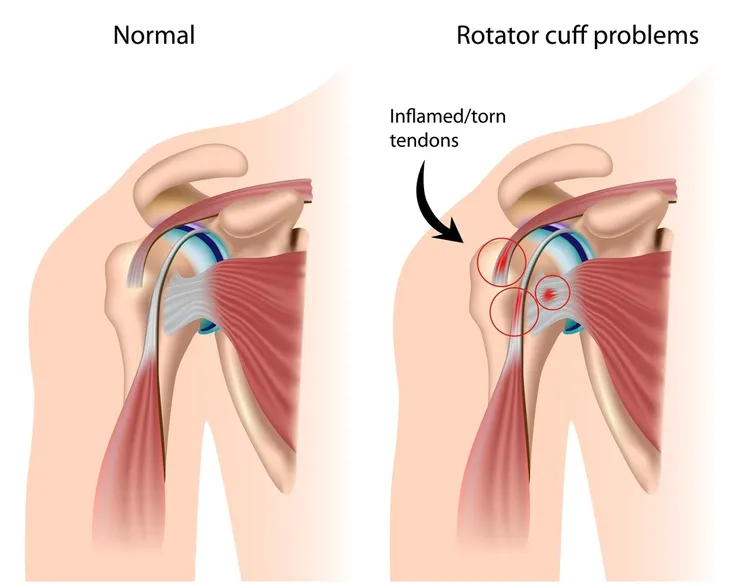
As mentioned earlier, sports and other activities that have repeated motions can be a risk for developing tendinitis. Because of this, you’re likely to develop the problem in your shoulders (both swimmer’s shoulder and pitcher’s shoulder come to mind).
However, you may also experience tendinitis in the knees, elbows (i.e., golfer’s elbow), heels, or wrists, notes Healthline. It notes that, while repetitive motion is a cause, the risk of developing tendinitis increases when you’re doing movements incorrectly, which can put additional strain on a tendon.
It Feels Worse Doing Activity
When you get pain in the area of a joint, you might mistake it for arthritis, bursitis, or something else. However, while you might feel a dull ache when resting, tendinitis typically flares up when you’re active. There may be a feeling that “the tendon is crackling or grating as it moves,” explains Medical News Today.
Other telltale signs include swelling or heat in the affected area, and there might also be a lump that forms along the inflamed tendon, adds the source. In more serious cases, a ruptured tendon could make movement more difficult.
Non-Sports Activities Can Cause It
If you think only repetitive motion during sports, such as baseball, tennis, and golf, or high-impact exercises are what leads to tendinitis, you should think again. The Cleveland Clinic explains that other popular activities you thought were relatively harmless, such as gardening and woodworking can cause the issue.
These activities, along with shoveling and painting, involve repetitive movements that are the basis for tendinitis. However, the clinic notes that even poor posture can be a risk factor.
It Might Be a Result of Your Occupation
The Mayo Clinic says job-related activities can lead to tendinitis if you’re not careful. Pay particular attention to proper technique if your job requires repetitive motions, requires you to be in “awkward positions,” or causes you to frequently reach up. Vibrations and “forceful exertion” can also be risk factors.
For example, while construction workers might be at risk of developing tendinitis due to performing manual labor, those working on assembly lines might also be at higher risk too. Even artists (painters in particular) and hairdressers can experience forms of tendinitis from repeated motions.
There are Non-Movement Risk Factors
The Cleveland Clinic notes that being over age 40 can raise your chance of developing tendinitis, as tendons tend to get less elastic with time. It notes that certain conditions, such as rheumatoid arthritis, can be a factor, as it can weaken muscles over time. It also mentions gout and diseases of the blood/kidney as being risks.
Meanwhile, the site also warns that certain medications can make you more prone to tendinitis. These medicines “that can cause tendons to tear” include fluoroquinolone antibiotics and statins (the latter is prescribed to manage cholesterol).
The Symptoms Can Be Gradual or Sudden
The Cleveland Clinic says that, while the main symptom of tendinitis is pain at the site of the tendon (and the surrounding tissue), it may come on gradually from minor strain. However, it sometimes sneaks up a lot quicker.
For example, a “sudden, more serious injury” can cause tendinitis, and it could come on suddenly in a severe way if there are calcium deposits present. Meanwhile, WebMD notes this form called calcific tendinitis is more common among women, and commonly affects the shoulders.
A Physical Exam and Imaging Can Diagnose It
If you’re experiencing pain around the joints, then it’s time for a visit to the doctor. They can assess your medical history and perform a physical exam focusing on the affected areas, explains Healthline. They will likely check for any tender areas and also test your range of motion.
The site says you should come prepared to share any helpful information that can aid in the diagnosis, such as whether you had any past injuries in the joint. The doctor will likely ask you about your current activities, and make use of imaging scans, such as X-rays or MRI, if there’s nothing conclusive.
Treatment Can Include Surgery
Healthline outlines a number of home strategies you can try to manage tendinitis. For example, you can simply put your feet up or apply ice or heat to the affected area. Non-prescription painkillers can also provide temporary relief.
Other approaches include using a compression wrap to reduce swelling and, in more extreme cases, using other supports such as braces or even a cane. While corticosteroid injections may also be another effective solution (but not a long-term one), you may need surgery to remove the inflamed tissue.
Keeping Tendinitis Under Control
If you are having symptoms of tendinitis, it’s important to address it early to avoid major issues, such as a tendon rupture requiring surgical repair, adds Healthline. The condition tends to resolve quickly when you deal with it sooner. Of course, avoiding getting to the point of discomfort in the first place is the most ideal path.
Healthline suggests you can do this by building muscle tone and warming up before exercise (although the jury is out on whether stretching before exercise will prevent tendon injuries). If you have a job where you have to sit in one place for long periods of time, be sure to get up and move around once in a while. If your tendinitis flares up, stop what you’re doing and take a 20-minute break to ice it.