According to doctors, a fatty liver isn’t damaging to the body on its own accord. However, the accumulation of excessive fatty tissue can lead to severe liver damage, including inflammation and scarring.
A fatty liver occurs when you take in more fat and calories than your liver can process. As a result, simple fats build up in the liver cells, making the liver prone to damage. The most common reason for the development of fatty liver disease is obesity, with obese individuals increasing their chances of developing the condition by about 75-percent. Although a fatty diet and weight gain is the main culprit, diabetes, hyperlipidemia (or elevated lipids in the blood), and alcohol abuse (with 90 to 100-percent of binge drinkers contracting fatty livers) will also increase the chances.
Here are the 15 most common symptoms of fatty liver disease…
1. Fatigue
If any organ in our bodies becomes dysfunctional, in this case the liver, the body will try to protect itself and compensate by pumping excess blood to the organ, which often leads to unexplained weakness, confusion, impaired judgment, or trouble concentrating; severe energy loss; and a sudden inability to participate in social activities that were once enjoyed. Researchers also speculate that changes in brain chemistry and hormone production contribute to feelings of fatigue and exhaustion.
The pathophysiology of liver disease-related fatigue often presents with additional neuropsychiatric symptoms, which typically develop over a compressed period of time. These symptoms can include problems such as depression and anxiety, which may be worsened by changes in your body’s ability to produce serotonin, an important mood regulator. Serotonin production can diminish in patients with fatty liver disease, leading to noticeable changes in mood. However, the root cause of these problems is frequently misdiagnosed, as clinicians may not immediately attribute them to liver problems.
2. Obesity
Doctors attest that carrying around a lot of excess weight will increase your risk of fatty liver disease by a whopping 75-percent. In addition, the individuals most prone to the condition are middle-aged, which means if you’re overweight and in your 40s or 50s, it’s in your best interest to adopt a healthier diet and get some regular exercise in effort to shed unwanted fat cells.
Liver problems can also interfere with your body’s ability to digest food and absorb nutrients, which can also lead to changes in weight. A chronically poor diet with a sustained intake of fatty, sugary, and/or salty foods is one of the root causes of fatty liver disease. If lifestyle factors such as poor diet or excessive alcohol intake are increasing your risk of developing liver problems, you should adopt healthier habits as soon as possible to reduce your chances of the serious health problems that can result.
3. Genetics
Heredity, something that’s passed down from parent to child, is often a primary indicator of future health problems. For instance, if a biological parent or grandparent was affected by liver disease, the children and grandchildren of that individual may also be stricken with the condition as well. In the case of liver disease, studies show the individual may be prone to obesity or alcoholism or be born with low levels of liver enzymes, which are involved in the metabolism of fats and alcohol.
If you are genetically predisposed to fatty liver disease or other types of liver problems, it’s especially important to be proactive about maintaining good health. Reduce or eliminate your consumption of alcohol and avoid overusing acetaminophen, as it can cause liver damage. Eat a healthy, balanced diet that limits sugar, salt and fat and make sure you’re eating plenty of fresh fruits and vegetables.
4. Jaundice
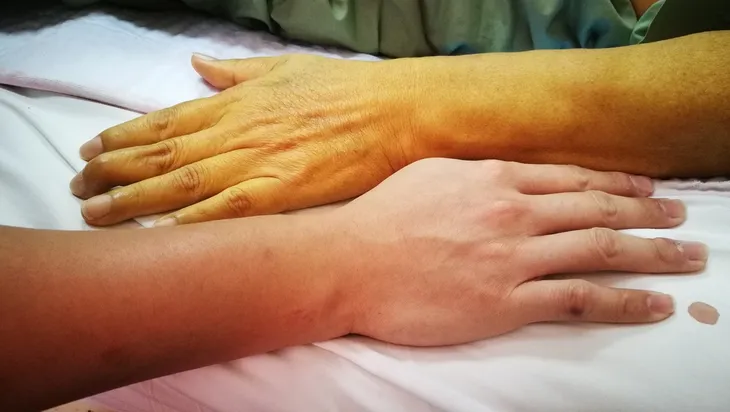
Jaundice, a condition characterized by yellowing of the skin and in the whites of the eyes is a common sign of liver disease. Jaundice is caused when bile flow from the liver is blocked, which brings out itchy, tiny yellow bumps around the eyelids and on the skin’s surface. These yellow deposits are caused by excess levels of bilirubin in the blood, which cannot be excreted from the body due to diminished liver function.
Clinicians classify jaundice in three different ways: hemolytic, hepatocellular, and cholestatic. Hemolytic jaundice indicates that the condition is arising outside of the liver and is likely caused by an infectious disease, such as malaria. Hepatocellular and cholestatic jaundice both occur within the liver, and doctors perform differential diagnoses to detect the exact cause of jaundice and determine whether or not it’s occurring as the result of diminished liver function.
5. Urine Color
Oftentimes, if jaundice develops, you will also notice changes in the color of your urine, which will usually appear unusually dark. This is because of the presence of toxins, which are normally processed by the liver, are passed through to the urine when the liver cannot properly deal with them. You may also notice that your urine has an unusually strong or pungent odor, and urination may become labored or painful as it thickens in consistency.
Changes in the constitution and color of your feces may also occur. Stools may become whitish or clay-colored, omitting a severe odor. Alternately, they could become tarry, and you may detect small or large amounts of blood when you pass a bowel movement. Such symptoms are serious and should be reported to your doctor immediately.
6. Skin Changes
In addition to skin changes due to jaundice, you may notice patchy skin and discoloration in the neck area (due to swollen glands) and under the arms once liver failure sets in. Additional skin alterations may show themselves in broken blood vessels on the face or spider veins on the chest, back, and shoulders. The hands can also be affected, with palms turning red and nail beds turning white with enlarged fingertips. In most cases, skin changes caused by fatty liver disease cause the skin to darken.
If you drink alcohol, you may notice that any such changes in your skin color intensify after periods of heavy drinking. You should interpret this as a serious sign that it’s time to make some significant lifestyle changes. Giving up drinking can be difficult, so if you’re struggling to ban the bottle, tell your doctor. He or she can direct you to medical and community-based resources that can make it easier for you to give up drinking for good.
7. Abdominal Pain
Abdominal pain may indicate liver disease or liver failure. You’ll experience the discomfort in the center or right upper portion of the abdomen, which may indicate internal bleeding. This may cause vomiting with tinges of blood occurs if blood vessels within the gastrointestinal tract become inflamed and rupture, and you may also notice blood in your stool. In many cases, abdominal pain will be accompanied by fluid retention in the stomach area, a condition known as ascites.
Ascites can be treated in numerous ways. First, your doctor will likely prescribe a diuretic, which is a type of drug that stimulates urination and encourages your body to rid itself of excess fluids. However, more aggressive treatments may be necessary if diuretics don’t relieve the condition. The abdominal pain associated with fatty liver disease may linger even if accompanying ascites is successfully treated, so keep a close eye on your symptoms and report them to your doctor during subsequent visits.
8. No Symptoms
Fatty liver disease is often called a silent killer—meaning it shows almost no symptoms, particularly in the beginning stages. However, should the disease be allowed to advance untreated over a number of years, with no signs, symptoms, or complications while fat accumulates, the liver will become inflamed and scarring will occur on the organ’s surface. Eventually, untreated fatty liver disease can lead to liver failure.
Because of the dangerous nature of fatty liver disease, it is very important for at-risk people (and everyone else, for that matter) to be proactive about prevention. There are many things you can do to reduce your risk for fatty liver disease. Yo-yo dieting, resulting in rapid, unchecked weight loss (often followed by a period of weight gain) is a leading cause of fatty liver disease. Excessive alcohol consumption and obesity are also linked with an increased risk of developing the condition. Living a moderate, healthy lifestyle will go a long way to safeguarding your long-term health.
9. Fluid Retention
An engorged abdomen, a condition called ascites, which occurs due to fluid retention in the abdomen and liver, will occur with the onset of severe liver disease. Ascites leads to an engorged, tight abdomen and a navel that appears pushed out due to fluid retention. It can also cause breathing challenges due to severe pressure on the internal organs.
While you’ve already learned about the treatments for ascites, you should also keep in mind that the fluid retention symptoms associated with fatty liver disease aren’t always limited to the stomach and abdomen; they can also occur in the lower legs, ankles and feet. This happens because of the natural action of gravity, which draws excess fluid down into the lower regions of the body. Again, diuretics will likely help, but you’re going to have to address the root cause to solve this problem permanently.
10. Muscle Wasting
People with advanced liver disease will often develop muscle wasting or another associated condition called Dupuytren’s contracture, in which the tendons in the hands shrink, fingers curl, and muscle tremors (or uncontrolled shaking) set in. This wasting away of the muscles comes from the liver’s diminished ability to metabolize proteins and can also make the patient more susceptible to fractures.
Patients will not normally experience these symptoms until the disease has reached an advanced and serious stage. However, it is usually preceded by rapid and unexplained weight loss, which in and of itself can have numerous causes. If you notice that you’re losing a lot of weight and haven’t made any major changes to your diet or exercise routines, it’s a good idea to visit your doctor to find out what’s going on. Remember that weight loss isn’t always a good thing and can signal the presence of an underlying disease or medical condition.
11. Confusion
As mentioned earlier, confusion may occur as a result of the body pumping excess blood to the liver in an attempt to protect itself. It’s not the only potential cause of confusion; however, it may also be a sign that there’s a build up of toxins.
Such a build up can occur because the impaired liver cannot metabolize and expel toxins as it normally would. As a result, they get into the bloodstream and are carried to the brain, leading to confusion, disorientation, and, in serious cases, coma. If any of these symptoms occur, it’s important that you make an appointment with your doctor as soon as possible.
12. Bleeding More Easily
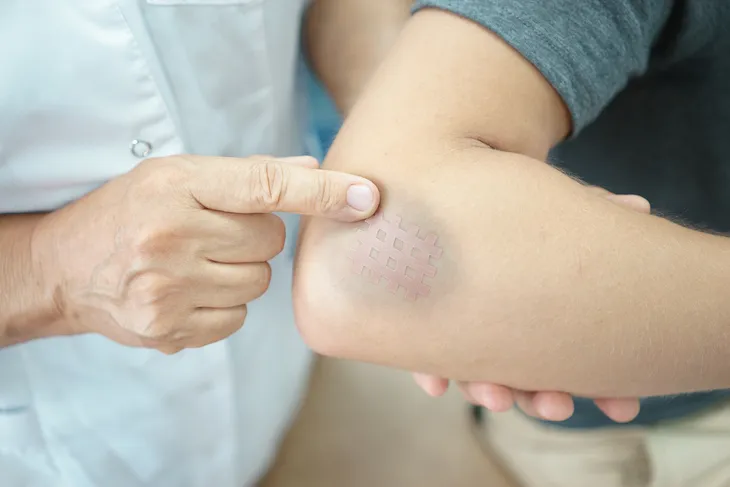
In addition to skin discoloration, such as jaundice, it was previously said that a person with fatty liver disease might notice broken blood vessels. However, before breaking they can appear quite enlarged just below the surface of the skin. This occurs due to pressure, which can come from carrying excess weight (obesity) and fluid retention, as were mentioned earlier.
This pressure makes the vessels very fragile, and susceptible to rupturing. As a result, people with liver disease can bruise easily. And should they injure themselves in a way that breaks the skin’s surface, excessive bleeding is common and occurs because the dysfunctional liver cannot make the proteins necessary for blood clotting.
13. Enlarged Breasts in Men
Men with fatty liver disease can develop larger than normal breasts, which is known medically as gynecomastia. One reason this can occur is because the impaired liver is unable to properly metabolize hormones like estrogen.
Men whose liver disease is caused by alcoholism are especially susceptible to gynecomastia, as alcohol can affect how the body synthesizes testosterone. And the phytoestrogens in alcohol can increase the body’s levels of this hormone, throwing off the ratio of estrogen to testosterone.
14. High Cholesterol
High levels of either triglycerides or LDL (“bad”) cholesterol in the blood can be indicative of excess fat in the liver. This can occur because, as Reader’s Digest explains, “The liver makes cholesterol on its own and circulates it into your bloodstream, but when we eat foods high in saturated and trans fats, it releases more fat and raises cholesterol levels.”
It’s important to get your cholesterol levels checked frequently, as having high cholesterol may not only be a sign of fatty liver disease but also a major risk factor for a variety of other serious health concerns, including heart disease and stroke.
15. High Blood Pressure
Your cholesterol may not be the only thing that’s higher than normal if you have fatty liver disease; high blood pressure is also common. In fact, a study conducted by German researchers found that people with non-alcoholic fatty liver disease (NAFLD) were “three times more likely to have hypertension than those who didn’t have the disease,” says Reader’s Digest.
Therefore, it’s important to have your blood pressure regularly checked, especially if you suspect that you may have fatty liver disease, as “Cardiovascular problems are the leading cause of death in people who have NAFLD,” says Dr. Malhi in speaking with the source.