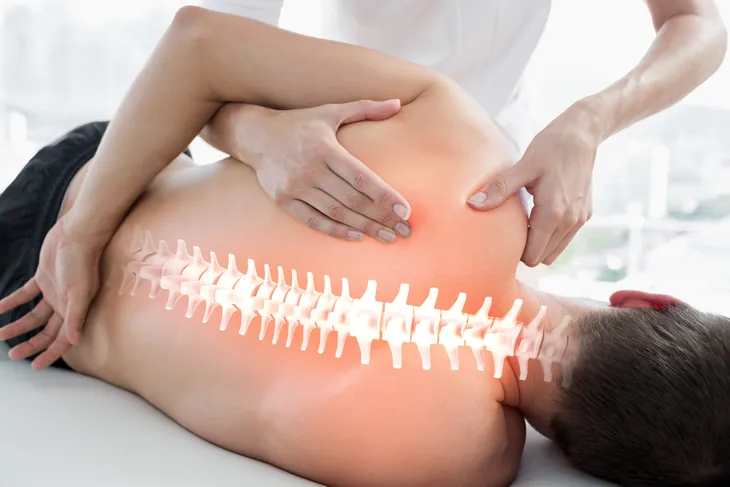
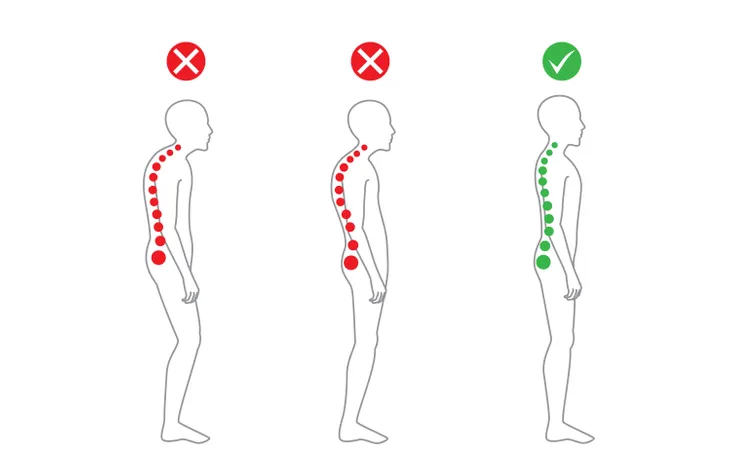
Ankylosing spondylitis is a bit of a tongue-twister to pronounce, but in layman’s terms, it is a type of arthritis that affects the human spine. It can be quite painful and results in a stooped-over posture (or more extreme spinal deformity) if left untreated.
Unlike its name, this article offers a simple and clear breakdown of what ankylosing spondylitis is, what causes it, how to identify it, and what can be done to treat it. Check it out…
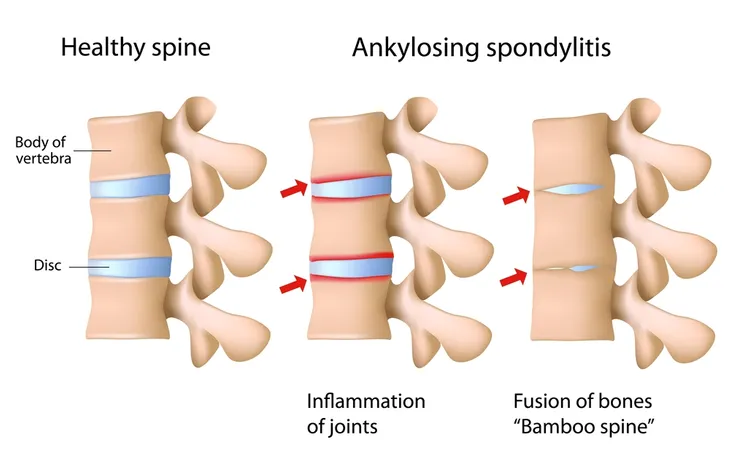
What Exactly is Ankylosing Spondylitis?
Ankylosing spondylitis occurs when some of the vertebrae (spinal bones) begin to fuse together. This is not supposed to happen and results in a very rigid spine. Luckily, early diagnosis and treatment can go a long way to reduce pain, serious spinal damage, or physical deformity.
Who Gets Ankylosing Spondylitis?
This condition is fairly rare, affecting only 0.1 to 0.5-percent of the adult population. It is slightly more prevalent among men in their teens and 20s, although it can affect both male and females. Women typically have milder cases of ankylosing spondylitis than men do. The condition is also more common in some Native American tribes, which is something to be aware of if you fall into that demographic.
Symptoms
There are a variety of symptoms, which can sometimes help with discovering the condition at an early stage.
Pain and Stiffness
As you would expect from an arthritic illness, ankylosing spondylitis will cause constant stiffness and soreness in the lower back, butt, and hips. If you experience this for a prolonged period (3-months or more), you should consult a doctor. The condition usually starts in the sacroiliac joints, which is where the lowest major part of your spine (sacrum) joins the pelvis (ilium bone) in your lower back.
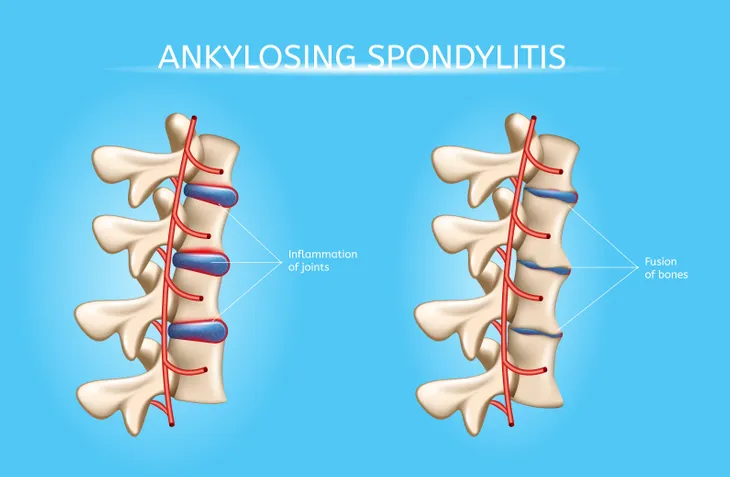
Bony Fusion
Ankylosing spondylitis can cause spinal bones to overgrow, which results in an abnormal fusion of bones that aren’t supposed to join. This is called bony fusion and can affect multiple areas of the body. Fusion in the neck, back, and hips can cause pain and impair your ability to perform normal daily activities. Fusion of the ribs (to the spine or breastplate) can inhibit breathing.
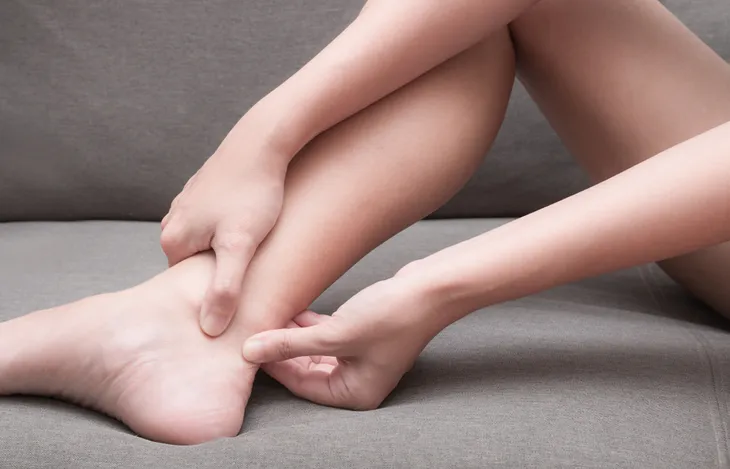
Pain in Ligaments and Tendons
Although ankylosing spondylitis is technically a spinal condition, it can affect other areas of the body. It can lead to tendinitis near the heels of your feet, especially behind or beneath the heel and in the Achilles tendon area.
Other Symptoms
Less common symptoms of ankylosing spondylitis include fever, constant fatigue, loss of appetite, eye inflammation (redness and pain), and in very rare cases, lung or heart problems may also develop.
What Causes Ankylosing Spondylitis?
There is no definite known cause for ankylosing spondylitis, other than it being strongly linked to genetics. Almost everyone who ends up with the condition also carries a certain gene, known as HLA-B27. This specific gene does make ankylosing spondylitis more likely, but it’s also not a sure thing. As many as 10-percent of the people who carry this gene never show any signs of the disease at all.
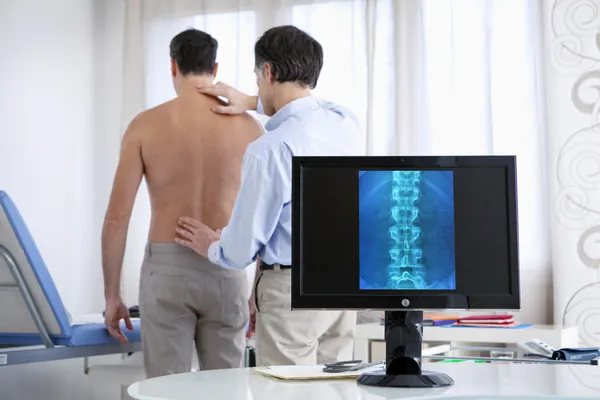
How To Diagnose Ankylosing Spondylitis
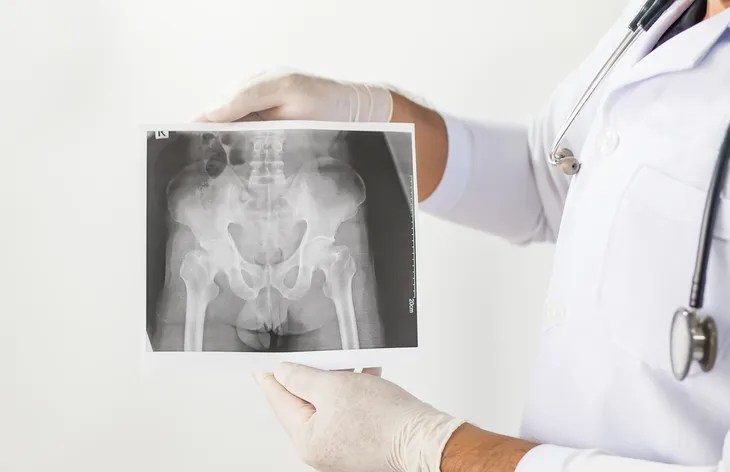
There’s no real surprises when it comes to diagnosing ankylosing spondylitis. The first clue will be the symptoms, which were listed previously. After that, a doctor will perform a physical exam and order X-rays of the back, pelvis, and possibly the rib area. A doctor will also perform chest measurements during breathing and conduct lab tests. After all of that, your doctor will be able to make a confident diagnosis.
Treatment
Group Approach
Although ankylosing spondylitis has no known cure, there are a variety of treatment options to reduce pain and discomfort and prevent it from getting worse. Proper treatment can reduce stiffness, help you maintain good posture, prevent spinal deformity, and basically keep you living a normal lifestyle.
The best form of treatment is a “group approach,” featuring a bunch of different health professionals working together, including a doctor, physical therapist, occupational therapists, and maybe even a surgeon.
Therapy and Exercise
Regular physical and/or occupational therapy will help maintain normal range of movement and body functionality.
Outside of physical therapy sessions, patients with ankylosing spondylitis should strive to get daily exercise, as it will reduce stiffness, and strengthen muscles. In addition, the deep breathing that comes with exercise will help keep the chest cage from getting stiff. If there is pain in a patient’s joints (especially the heels), swimming is a great form of exercise for those with ankylosing spondylitis.
Medications and Surgery
There are a variety of medications you can take to counter ankylosing spondylitis. In basic cases of the disease, nonsteroidal anti-inflammatory drugs (NSAIDs) are typically used. Ibuprofen (Advil), naproxen (Aleve), and aspirin are examples of NSAIDs. In more serious cases, stronger prescription drugs may be recommended.
Newer drugs have also been found effective to reduce pain and stiffness. Biologics, such as adalimumab (Humira), adalimumab-atto (Amjevita), certolizumab pegol (Cimzia), etanercept (Enbrel), etanercept-szzs (Erelzi), infliximab Remicade), and infliximab-dyyb (Inflectra) have all been approved by the US Food and Drug Administration (FDA) for the treatment of ankylosing spondylitis.
Always consult your doctor as to which medication might be the right choice for your specific condition and needs. In some cases, steroid injections into the joints or tendons can also be useful.
Some patients may opt for artificial joint replacement surgery, although it is typically used in the hip and knee joints and not the spine.
Other Recommendations
People with ankylosing spondylitis should not smoke or use chewing tobacco, as it can aggravate and accelerate the condition. Additionally, patients are urged to sleep on a firm mattress to keep the spine straight, and even to use thin pillows so that the neck doesn’t rest in the forward “flexed” position overnight. Propping up your feet or legs overnight (with pillows or blankets) is also a no-no, as it can lead to increased bone fusion in the hips or knees.
You should carefully choose where and how you sit if you are suffering from ankylosing spondylitis. Make sure that your office chair (if you use one) is ergonomically correct and offers good support. Chairs with armrests are preferred over chairs without them, and of course, sit up straight! Practicing proper posture will go a long way to prevent soreness and stiffness.