The thermometer is dropping as winter approaches, and some people may feel it more than others, especially in their fingers and toes. That’s because they may have a condition called Raynaud’s disease (also called Raynaud’s syndrome or phenomenon) that causes numbness and other symptoms in the extremities when it gets colder.
While your fingers can go numb and change color when exposed to extreme cold for prolonged periods of time (commonly known as frostbite), those with Raynaud’s (up to 10-percent of Americans) can suffer uncomfortable symptoms, even when the indoor or outdoor environment isn’t very cold. Here are eight cold, tingling facts about this health problem…
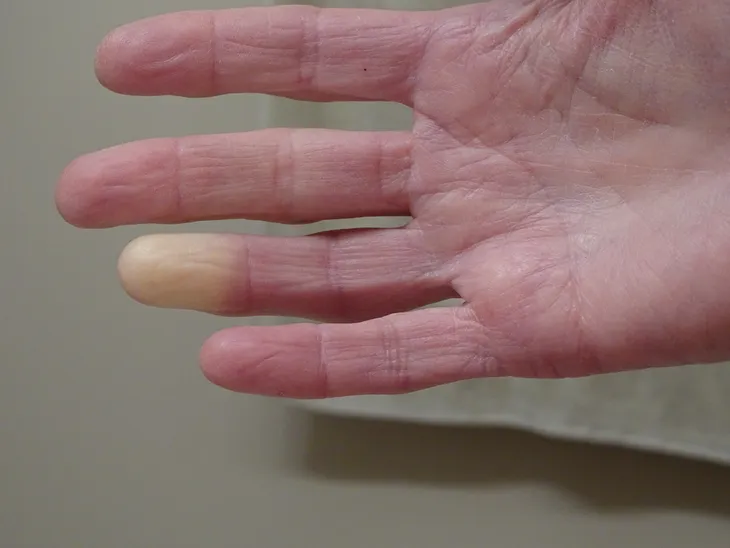
1. White Fingers First
The Mayo Clinic explains that during an “attack” of Raynaud’s disease, a patient’s fingers usually turn white first (which is actually what happens during a more advanced stage of frostbite). Then, the skin will often turn blue while feeling cold and numb.
“As you warm and circulation improves, the affected areas may turn red, throb, tingle, or swell,” says the clinic. This is the opposite of frostbite, as the skin will turn red first before turning white, and defrosting from frostbite can also be quite painful.
2. Women are More Affected
According to Raynauds.org, women are more likely to have this health problem. Apparently, women between the ages of 15 and 30 are most affected.
This probably won’t come as any surprise, but women who live in colder climates, for example, further north in the U.S., will have this problem more often than those who aren’t exposed regularly to colder climates.
3. There are Two Types
The National Heart, Lung, and Blood Institute explains there is primary and secondary Raynaud’s disease, and the latter version is actually more severe. The cause of primary Raynaud’s disease isn’t known, but it’s the more common of the two types.
Meanwhile, secondary Raynaud’s disease is caused by an underlying health condition, such as those that affect the arteries or nerves associated with arteries in the hands and feet. It can even be caused by a repetitive movement injury or exposure to certain chemicals.
4. Warm Water Rescue
Unlike frozen fingers with frostbite, dipping your hands in warm water when you have an attack of Raynaud’s can provide some relief, according to the Raynaud’s Association. Trying this with frostbite before circulation has returned can actually cause more damage to tissue.
The association said another strategy, if you’re having a Raynaud’s attack, is to move your hands and feet to increase blood flow “and to rub them where they are sore to help with circulation.”
5. It Can Be Triggered by Stress
Cleveland Clinic explains that while the cold is the biggest culprit when it comes to triggering a Raynaud’s attack, it can also be brought on by emotional stress.
Whether it’s from cold temperatures or stress, Raynaud’s closes the blood vessels that supply the finger and toes more than the natural response should allow. Excitement can also lead to a Raynaud’s attack.
6. It Affects More than Fingers
While the disease is most commonly associated with affecting the fingers and toes, Raynaud’s can actually strike a number of other sensitive areas of the body, explains MedicalNewsToday.com.
Other areas of the body that can be affected by a Raynaud’s attack include the nose, lips, and ears. Some women may experience Raynaud’s of the nipples, which can be pronounced during breastfeeding and cause a lot of discomfort. “It causes severe throbbing, similar to that experienced with a fungal Candida albicans (C. albicans) infection, which can lead to misdiagnosis,” adds the source.
7. It Can be Triggered by Medications
NHS in the UK explains that secondary Raynaud’s can actually be caused by certain medications, including certain types of anti-migraine medications (such as sumatriptan [Imitrex] and ergotamine [Cafergot]). Beta blockers used to control high blood pressure can also be a trigger.
The source continues by warning that certain decongestants and even birth control pills could be the cause of secondary Raynaud’s. It’s probably best to consult with a doctor to assess medications and see if any can be adjusted or changed to eliminate the problem. Illegal drugs such as cocaine, have also been known to trigger attacks.
8. There are Medical Treatments
While some medications may cause secondary Raynaud’s, other drugs may help alleviate the issue, according to the Mayo Clinic. The source says your doctor may prescribe calcium channel blockers (including nifedipine [Procardia]) to relax and open small blood vessels, while vasodilators, including nitroglycerin cream, can help.
Other sources say non-prescription pills, namely vitamin B-3 (niacin) pills, can help naturally increase blood flow and reduce the unpleasant symptoms of Raynaud’s. It’s always best to check with your doctor before following through with a drug or non-drug solution.