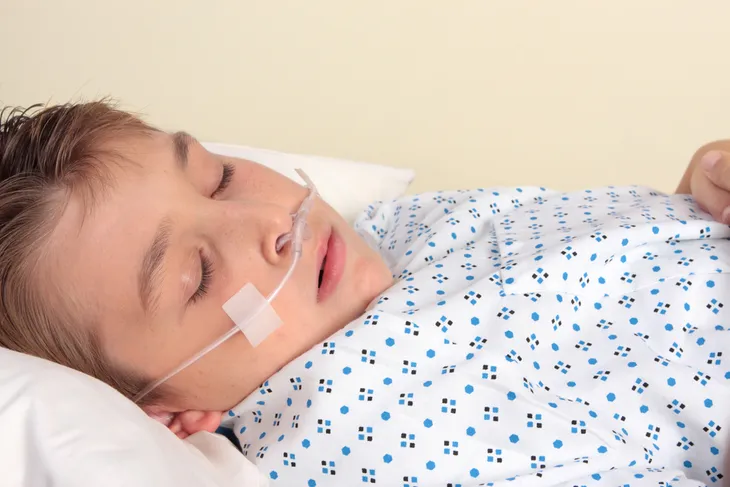
Also known as LGS, this syndrome affects younger children (starting between ages two to six) and is a rare form of epilepsy, according to WebMD. This results in frequent seizures of varying forms, adds the source.
WebMD also notes the condition is especially difficult to treat, however research is ongoing. There can be other symptoms related the syndrome, such as learning difficulties and development delays, it adds. Here are six possible explanations for the medical problem…
1. Lack of Oxygen
DoveMed.com notes that a reduced oxygen supply to a baby, also referred to as perinatal hypoxia, can be a risk factor for LGS. Other sources break down the reasons why an infant may not be getting sufficient oxygen immediately before and after birth – for example, a traumatic birth could temporarily cut off air supply to a newborn, killing off some essential brain cells.
Infants can also experience a higher risk of perinatal hypoxia if the mother smokes, the mother has anemia, or there’s a traumatic brain injury, according to BirthInjuryGuide.org.
2. Infections
AboutKidsHealth.ca explains that infections of the central nervous system might be responsible for the seizures associated with Lennox-Gastaut Syndrome. Degenerative and metabolic disorders of the nervous system could also be to blame, it adds.
Among these infections and genetic metabolic disorders are meningitis, which is characterized by inflammation of the brain and spinal cord’s protective membranes, as well as tuberous sclerosis, a rare condition that causes non-cancerous tumors to form throughout the body.
3. Family History
As mentioned earlier, genetics can come into play when it comes to triggering this syndrome. AboutKidsHealth.ca explains that between three and 27-percent of children with LGS have a family history of epilepsy.
That being said, the source also notes about 30-percent of cases of LGS have no obvious underlying cause (cryptogenic). The patients that fall into this cryptogenic category are more likely to have a family history of epilepsy than children with a symptomatic version of the syndrome (arising from another underlying cause).
4. History of Infantile Spasms
While a child’s family history might come into play regarding risk levels for developing LGS, their own health history can be a factor too, notes DoveMed.com.
The source explains that approximately 17 to 30-percent of LGS patients have a prior history of “infantile spasms” (also known as epileptic spasms or juvenile spasms) that is a rare condition that occurs in children under a year old. It also adds, “Individuals with a history of infantile spasms often have a more severe prognosis with LGS”.
5. Cortical Dysplasia
WebMD said while brain infections such as meningitis can be an underlying trigger of LGS, so can a condition called cortical dysplasia, “where some nerve fibers in the brain don’t line up right during development in the womb,” it explains.
Cincinnati Children’s Hospital Medical Center says this condition is “one of the most common causes of epilepsy,” and that the most common form of cortical dysplasia is focal cortical dysplasia, which itself has 3-types. One of the types is severe and is more common in children, affecting the frontal and temporal lobes of the brain, it adds.
6. Brain Malformations
Several sources say that brain malformations can be responsible for LGS, which could also account for some learning challenges in the young children. MedicinePlus.gov explains that most brain malformations “begin long before a baby is born”.
Brain malformation means the brain may be an abnormal size, or be missing parts altogether, explains the site. It can be from genetic factors, but also from exposure to certain medications or radiation during pregnancy, it adds.