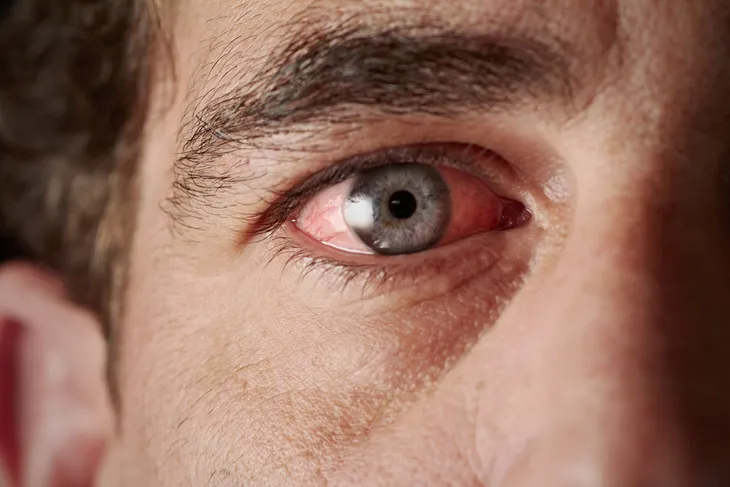
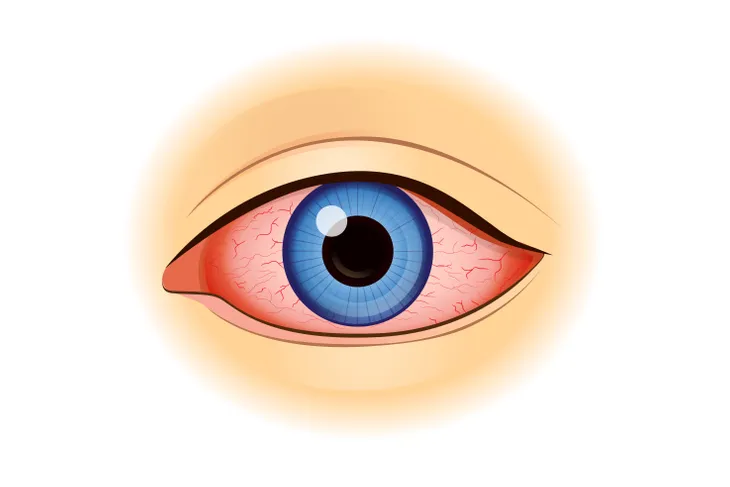
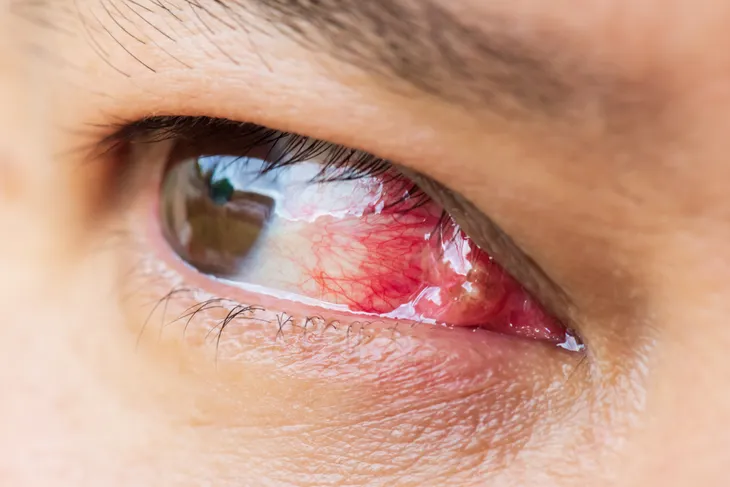
Red eye is a sign of eye inflammation and can occur in one or both eyes. It occurs when blood vessels in the eye become swollen or irritated and can affect any part of the eye. It is one of the most common eye ailments seen by primary care physicians and has a multitude of causes. Red eye is an alarming condition and the majority of cases represent minor eye problems. But some cases may be serious and require emergency medical evaluation. The most serious cases of red eye may be accompanied by eye pain or changes in vision.
Twelve causes of red eye are…
1. Infectious Conjunctivitis
Infectious conjunctivitis, also known as “pink eye”, is the most common cause of red eye. It is an extremely contagious infection, particularly among school-age children. Conjunctivitis represents inflammation of the conjunctiva, the thin layer of tissue covering the eyeball and inner surfaces of the eyelid. Bacterial or viral infection may cause infectious conjunctivitis. It may affect one or both eyes.
Classic symptoms of “pink eye” can include red eye(s), discharge from the eye(s), itchy or scratchy eye(s), excessive tearing, increased sensitivity to light, and crusting of eyelids or eyelashes. The most common viral cause in children is adenovirus. The most common bacterial cause in kids is strep. Treatment of bacterial conjunctivitis usually involves antibiotic eye drops or ointments. Antibiotics cannot cure viral conjunctivitis and it just has to run its course. The majority of cases of infectious conjunctivitis resolve without complication.
2. Subconjunctival Hemorrhage
Subconjunctival hemorrhage represents a burst blood vessel in the eye. Blood collects under the conjunctiva, the thin layer of tissue covering the eyeball and inner surfaces of the eyelid. The cause of a subconjunctival hemorrhage is not always apparent. Some common causes of this condition include violent coughing, powerful sneezing, vomiting, heavy lifting, and injury to the eye.
Risk factors for the occurrence of a subconjunctival hemorrhage include diabetes, high blood pressure (hypertension), blood-thinning medications, and blood-clotting disorders. Despite its alarming appearance, a subconjunctival hemorrhage is usually not accompanied by a change in vision, discharge from the eye, or eye pain. The condition is harmless (benign) and the body will reabsorb the blood in a few weeks. There are no known complications from this condition.
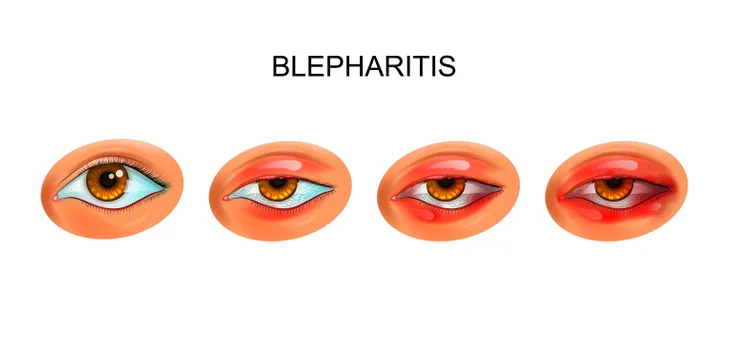
3. Blepharitis
Blepharitis is inflammation of the eyelids. It is often a chronic condition and usually involves the part of the eyelid where the eyelashes grow. The condition usually affects both eyelids. Clinically there are two forms of blepharitis: anterior and posterior. Anterior blepharitis affects the front of the eyelid from which the eyelashes arise. Posterior blepharitis occurs when oil glands located near the base of the eyelashes become clogged.
Blepharitis may be caused several diseases and conditions including dandruff of the scalp and eyebrows, bacterial infection, rosacea (a skin disease characterized by facial redness), allergies, and eyelash lice. Symptoms of blepharitis may include excessive tearing, red eyes, foreign body sensation, eyelash crusting, decreased vision, swollen eyelids, sensitivity to light, itchy eyelids, and loss of eyelashes. It can be a frustrating condition, but usually responds to warm compresses, washing the eyelid margins, and applying antibiotic ointment.
4. Dry Eye Syndrome
Dry eye syndrome is a common condition in the United States. It may be characterized by decreased tear production or the production of poor-quality tears. The condition is more common in women. Dry eye syndrome can inflame and irritate the blood vessels on the surface of the eye, leading to redness in the eyes. Other symptoms of dry eye syndrome may include burning, foreign body sensation, blurry vision, stringy mucus, eye fatigue, and sensitivity to light.
A number of factors can increase the risk of developing dry eye syndrome including increasing age, female gender, a diet low in vitamin A, wearing contact lenses, smoking, computer use, and some medications (antihistamines, antidepressants, and certain blood pressure medications). It has an association with some diseases such as Sjogren’s syndrome, diabetes, lupus, and rheumatoid arthritis. Effective treatment options for dry eye syndrome include cyclosporine (Restasis, an anti-inflammatory agent), artificial tears, or plugs to block the drainage holes in the corners of the eyes.
5. Stye
A stye, also known as a hordeolum, is a red, painful lump near the edge of the eyelid. It represents a bacterial infection and is usually filled with pus. A stye typically resembles a pimple or boil. Other symptoms of the condition may include redness of the eyes, eyelid pain, eyelid swelling, blurry vision, and excessive tearing. Staphylococcus, or “staph”, bacteria cause the majority of infections responsible for styes.
Styes are more common in adults than in children. Individuals with blepharitis, meibomian gland dysfunction, and rosacea (a skin disease characterized by facial redness) are at increased risk for developing styes. Meibomian glands secrete oil that lubricates the eyes. Most styes don’t require any specific treatment and resolve spontaneously in 1 to 2-weeks. If a stye requires treatment, eyelid scrubs, warm compresses, and an antibiotic ointment are usually effective.
6. Closed-Angle Glaucoma
Glaucoma is an eye condition characterized by increased pressure in the front (anterior) chamber of the eye. The two major categories of glaucoma are open-angle and closed-angle. Open-angle is the most common form of glaucoma and accounts for 90-percent of cases. Closed-angle glaucoma is much less common. If untreated or uncontrolled, glaucoma can lead to peripheral vision loss and eventually blindness. Glaucoma is the second-leading cause of blindness in the United States.
Closed-angle glaucoma may be primary or secondary. It can also be described as acute or chronic. Risk factors for this condition include advancing age, being farsighted, female gender, and Asian or native Alaskan descent. Symptoms of acute closed-angle glaucoma may include red eyes, eye pain, headaches, vision loss, halos around lights, blurry vision, nausea and vomiting, and dilated pupils. These symptoms signal a medical emergency. The definitive treatment for the condition is laser iridotomy, which involves a laser incision into the iris of the eye to decrease pressure.
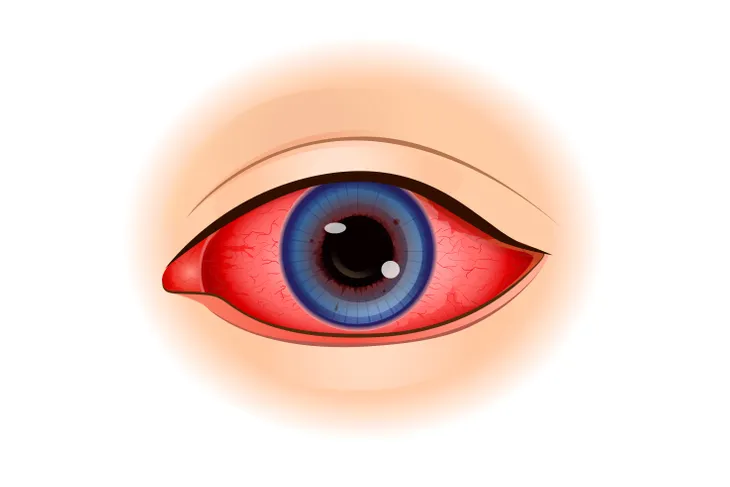
7. Uveitis
Uveitis is inflammation of the uvea, the middle layer of the eye. Uveitis may be classified as anterior (front of the eye), intermediate (middle of the eye), posterior (back of the eye), or panuveitis (all parts of the eye). It may affect one or both eyes. A specific cause cannot be determined in half of all cases of uveitis. Autoimmune diseases or infections may cause the remainder of the cases of uveitis.
Signs and symptoms of uveitis may include severe eye redness, eye pain, light sensitivity, floaters (dark, floating spots in the field of vision), and blurry vision. The goal of treatment is to reduce inflammation in the eye. Depending on the cause uveitis may be treated with steroids, antibiotics, antivirals, or drugs to suppress the immune system.
Potential complications of uveitis include cataracts (clouding of the lens of the eye), glaucoma (increased pressure in the eye), detachment of the retina (a medical emergency), and blindness.
8. Corneal Abrasion
A corneal abrasion is a scratch on the cornea of the eye. It is one of the most common eye injuries. The cornea is the transparent layer over the front of the eye covering the iris (the colored part of the eye) and the pupil (the black circle in the middle of the eye). The abrasion is typically limited to the most superficial layer of the cornea.
Possible causes of corneal abrasion vary and may include injury, extended contact lens wear, foreign matter being blown into the eyes, and not protecting the eyes during surgery while under general anesthesia. Symptoms of corneal abrasion may include eye redness, eye pain, foreign body sensation, excessive tearing, sensitivity to light, and blurry vision. Complications from corneal abrasion are rare, and most minor abrasions heal within 24 to 48-hours. Research has not shown any benefit from patching the affected eye.
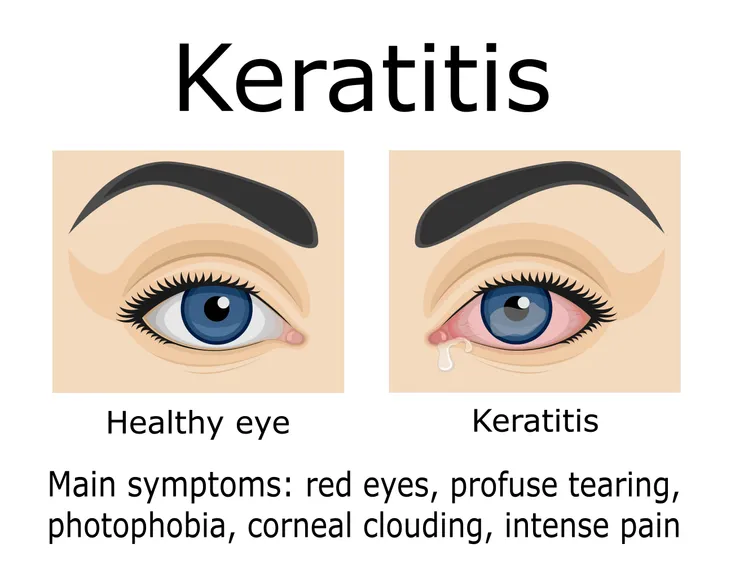
9. Keratitis
Keratitis is inflammation of the cornea, the transparent layer over the front of the eye covering the iris and pupil. It refracts light and focuses it toward the retina, the light-sensitive tissue layer at the back of the eye. Keratitis may be infectious or noninfectious. Infection is the most frequent cause of keratitis. Risk factors for the development of keratitis include wearing contact lenses, reduced immunity, living in a warm climate, using steroid eye drops, and injuring the eye.
Symptoms of keratitis may include eye redness, eye pain, excessive tearing, blurry vision, and sensitivity to light. Treatment depends on the cause of keratitis. Infectious keratitis generally requires treatment with antibiotic, antiviral, or antifungal agents. Steroid eye drops may be used short term to decrease inflammation and limit scarring of the cornea. Complications of keratitis may include corneal ulcers and scarring, which could lead to decreased vision and even blindness.
10. Allergic Conjunctivitis
Allergic conjunctivitis is inflammation of the conjunctiva (the thin layer of tissue covering the eyeball and inner surfaces of the eyelid) due to allergens. Common airborne allergens include dust, pollen, grass, weeds, pet dander (microscopic flecks of skin shed from pets), and mold spores. Allergic conjunctivitis is quite common and affects almost 20-percent of the population in the United States. There are two main types of allergic conjunctivitis: acute (seasonal) and chronic (year-round).
Symptoms of allergic conjunctivitis may include red, watery, itchy, and burning eyes. The symptoms of this condition are mediated by histamine, the same mediator of allergic rhinitis (hay fever). Histamine is produced by mast cells. The best treatment is avoidance of known symptom triggers. Allergic conjunctivitis may be treated with a variety of drugs including topical antihistamines, mast cell stabilizers, nonsteroidal anti-inflammatory drugs (NSAIDs), and steroids. The prognosis for this condition is excellent and there is no potential for serious complications.
11. Pterygium
A pterygium is a growth that develops on the conjunctiva (the thin layer of tissue covering the eyeball and inner surfaces of the eyelid). Pterygia may occur in one or both eyes and vary in size from small to very large. The growth is benign (noncancerous) and occasionally may extend to the cornea (the clear part of the eye that covers the iris and pupil).
Symptoms of a pterygium may include eye redness, swelling, itching, and blurring of vision. Risk factors for development of the condition include increased exposure to ultraviolet (UV) light and having an occupation that requires outdoor activities. Pterygia affect males more often than females (2:1 ratio). A pterygium usually doesn’t require any treatment unless it is obstructing vision or extremely uncomfortable. Treatment may consist of artificial tears, topical ointments, occasional short-term steroid drops, and surgical removal if needed.
12. Cluster Headaches
Cluster headaches are exquisitely painful headaches that occur in cycles, or clusters, followed by headache-free periods. Cluster headaches may be classified as episodic or chronic. The exact cause of cluster headaches is unknown, but researchers have observed widening of the blood vessels supplying the brain and face. Risk factors for cluster headache may include male gender, age older than 30-years, and excessive alcohol consumption.
The cardinal symptom of cluster headache is a one-sided headache, which may be accompanied by eye redness, excessive tearing, nasal congestion, runny nose, constricted pupil, drooping upper eyelid, facial sweating, and swelling of the eyelid. All of the accompany symptoms typically occur on the same side as the headache. Treatment of acute cluster headaches may entail breathing 100-percent oxygen, sumatriptan (Imitrex) administered nasally, or an injection of dihydroergotamine (DHE). Preventative medications may also be used to treat cluster headaches.