Diabetes, dubbed the “silent killer,” is a condition that affects millions of people across America. Type 2 diabetes, is the most common form of the disease, affecting approximately 90-percent of total diabetes sufferers. The only surefire way to diagnose diabetes is by getting your doctor to perform a fasting blood sugar test.
The following 15 symptoms can also be indicative of type 2 diabetes…
1. Reoccurring Infections
Type 2 diabetes causes those suffering from the condition to live in an immunosuppressed state, which ultimately leaves them susceptible to a variety of bacterial infections such as yeast (or Candida) infections, pneumonia, urinary tract infections (UTIs), and skin rashes. Basically, “immunosuppression” means that the immune system is unable to fight off infection.
Yeast infections are among the most common because high blood sugar creates an environment that is favorable for the growth of yeast. “Glucose is fuel for yeast. The more that’s around, the more they can multiply,” says Mary Vouyiouklis Kellis, MD, an endocrinologist at Cleveland Clinic to Women’s Health.
For the diabetic, infections are a constant concern since those suffering from the condition are more prone to developing infections due to high blood sugar levels wearing down the immune system and it’s ability to protect the body. Nerve damage, which also results from low blood flow to the extremities (i.e., legs, feet, arms, and hands) in some diabetic patients, can raise the risk of infection.
2. Increased Urination
An increase in the frequency and urgency of urination could lead a doctor to suspect diabetes. More often, frequent urination is a wake-up call that you have an underlying health condition, especially if that wake-up call interrupts your sleep multiple times a night.
This is due to the fact that individuals with type 2 diabetes have overactive kidneys that are working to eliminate excess glucose in the blood, and the fastest way to eliminate anything from the body is through urination. Keep in mind that this increased urine output may not only keep you up at night but also cause dehydration, so be sure to stay hydrated.
3. Increased Appetite
Unexplained hunger that comes in waves is mimicking the rollercoaster of blood sugar highs and lows that a person with type 2 diabetes commonly suffers from. A ravenous appetite occurs when blood sugar levels drop dangerously low, causing the body to demand glucose to function. Oftentimes, hunger pangs will come at unexpected times, even during the middle of the night.
Experts from the American Dietetic Association recommend upping the healthy fat and lean protein content of meals (i.e., nut butters, oil, avocados, raw nuts, etc.) so your body stays full for longer periods of time. Be sure to remember that you will burn through carbohydrates within a few hours, which is why hunger pangs are common mid morning and mid-afternoon.
For more tips on what to eat, check out our article on Type 2 Diabetes: Top Foods to Avoid.
4. Unquenchable Thirst
Excessive thirst often occurs with the onset of type 2 diabetes. This is how the body signals that it needs to replenish fluid levels lost due to more frequent urination and sometimes, perspiration.
As mentioned, it’s common for type 2 diabetics to have overactive kidneys, which is how the body attempts to eliminate excess glucose in the blood through urination. With increased bathroom breaks, the risk of dehydration is high, so be sure to hydrate regularly throughout the day. To make matters worse, many people don’t realize they have diabetes, so they will try to quench their thirst with sugary drinks, such as soda or juice, but these just increase the blood sugar and make things worse, explains Poorani Goundan, MD, an endocrinologist at Boston Medical Center, to Women’s Health. Always carry a water bottle and drink herbal teas rather than caffeinated drinks.
5. Exhaustion
Increased blood sugar levels cause frequent urination, immune suppression, and a general sense of not feeling well, as well as extreme exhaustion. This general discomfort from all the other symptoms, plus the draining effects that excess glucose elimination has on the body, will suck away any energy and cause a person to constantly feel like they need more rest.
Remember, as your body flushes out glucose via urination, it’s also flushing out vitamins, nutrients, and minerals from food before they can be absorbed. Let yourself rest when you feel tired to prevent an injury or to protect your already low immune system. “Carbohydrates, which your body breaks down into glucose, are your body’s main source of energy. But your body can’t effectively use that source of energy when you have diabetes,” writes Women’s Health after talking to Poorani Goundan, MD.
6. Sudden Weight Loss
Most of us would love to lose a few pounds here and there, particularly without much effort, but when weight loss is sudden and unexplained, it’s usually nothing to rejoice about. It’s often a sign that something more serious is going on. Diabetes is one of the serious conditions that can cause sudden weight loss. It occurs when specific hormone levels become unregulated and prevent the body from getting glucose from the blood into the body’s cells to use as energy. As a result, your body will begin burning fat and muscle for energy, which can often lead to sudden weight loss.
This sudden weight loss can occur as a consequence of high blood sugar, dehydration, muscle breakdown, and problems with your thyroid. Although this sudden weight loss is more common with type 1 diabetics, it can also strike type 2 diabetics several days after the onset of the condition. “Because you’re unable to get enough energy from sugar, your body burns your own fat and muscle for energy,” says Kellis to Women’s Health. “Weight loss can be pretty significant, sometimes 10 to 20-pounds.”
The general rule of thumb is to visit a doctor if you have lost between 5 and 10-percent of your body weight in the span of only 6-months.
7. Mood Swings
The glucose peaks and valleys experienced by type 2 diabetics will also leave you trapped on a never-ending roller coaster of emotion. When blood sugar is high, moods can be giddy and downright silly, but when blood sugar drops, your mood can turn to irritable and downright nasty until energy stores are replenished with food.
According to research, type 2 diabetics run twice the risk of developing depression, more so for female patients compared to male patients. Luckily, several healthy lifestyle changes that proactively improve diet, physical fitness, health, and wellness are a good way to prevent and ward off depression and mood imbalances.
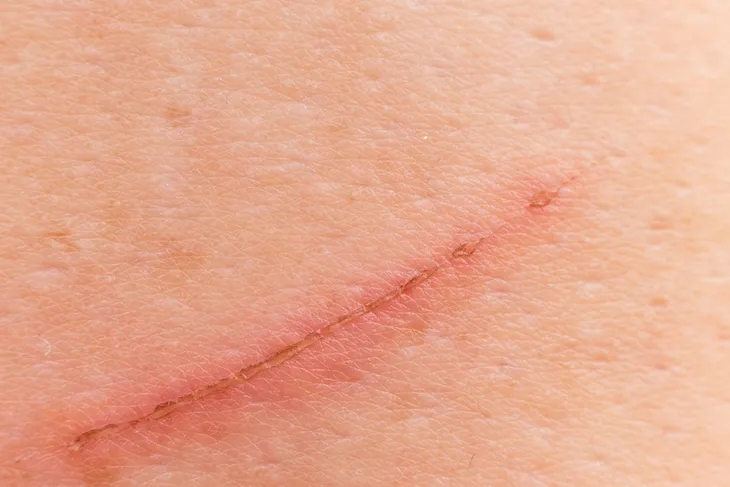
8. Slow to Heal
Due to blood vessel damage from increased glucose in the veins, type 2 diabetes sufferers often experience restricted blood flow, which causes a decrease in the time needed to heal surface abrasions, bruises, cuts, skin rashes, and infections. For type 2 diabetics, this slow rate of healing results from a lack of blood flow to the extremities. “High blood sugars provide a good environment for bacteria to grow,” says Poorani Goundan, MD, to Women’s Health.
High blood pressure and high cholesterol are common in diabetics which means there’s more chance for plaque buildup in the blood vessels. This means that cuts, bruises, burns, and abrasions that occur on the feet, legs, knees, hands, and arms get lower blood circulating to those areas, which slows healing. Fresh blood flow to any area is the body’s method to encourage the healing process.
Another reason cuts are slow to heal in diabetics is because they have limited sensation. “You’re less likely to notice a cut because you can’t feel it, which means you’re less likely to take care of it and it’s more likely to get infected,” says Dr. Goundan.
9. Numb Fingers and Toes
Chills, inflammation, tingling, and prickly numbness in the fingers and toes are other symptoms linked to type 2 diabetes. This discomfort occurs when excessive glucose in the body causes neuropathy (or nerve damage). High blood sugars will weaken and damage the nerve fibers all throughout the body, but for diabetics, the nerves in the feet and legs are the most prone to damage.
The effects of diabetic neuropathy are often reported as tingling, pain, or numbness in the extremities (usually the hands and feet), but can also extend to major systems and organs (i.e., the heart, urinary tract, digestive system, and even the blood vessels). Diabetic neuropathy can range from mild to disabling and potentially fatal. Unfortunately, if diabetes is left untreated, this neuropathy can be permanent.
10. Vision Problems
Vision is closely linked to blood sugar levels, which means when blood sugar drops, a person suffering from type 2 diabetes will experience blurred vision, floaters, and even light sensitivity. Luckily, once blood sugar is stabilized, vision will return to normal, but leaving blood sugar unbalanced for too long may permanently damage vision.
Diabetes-related eye issues develop when the condition is left untreated because vision problems are directly linked to blood sugar control. This means that when blood glucose levels are not managed adequately, the likelihood of eye issues will reduce for the diabetic will be reduced. According to a United Kingdom Prospective Diabetes Study, published by Diabetes UK, the threat of glaucoma and cataracts is double for diabetics vs. the general population. Both conditions can lead to blindness if blood sugars are not managed properly.
11. Strange Smelling Breath
We already talked about how diabetes leads to dehydration which causes an unquenchable thirst and a dry mouth. Well, this also leads to bad smelling breath. When the mouth is dry, there is no saliva to wash away the bacteria and balance out the pH in the mouth. “Undiagnosed or uncontrolled diabetes can trigger ketosis, a process in which the body uses fat, rather than glucose, for energy,” explains Women’s Health. “Ketosis releases a chemical byproduct called ketones, which can make your breath smell unpleasantly sweet or fruity.” It could even smell like acetone (which is a type of ketone), says Mary Vouyiouklis Kellis, MD, an endocrinologist at Cleveland Clinic, to the source.
If you notice that your breath is beginning to smell strange and you’re not on a ketogenic diet, then you should consult your doctor to find out what’s causing this change.
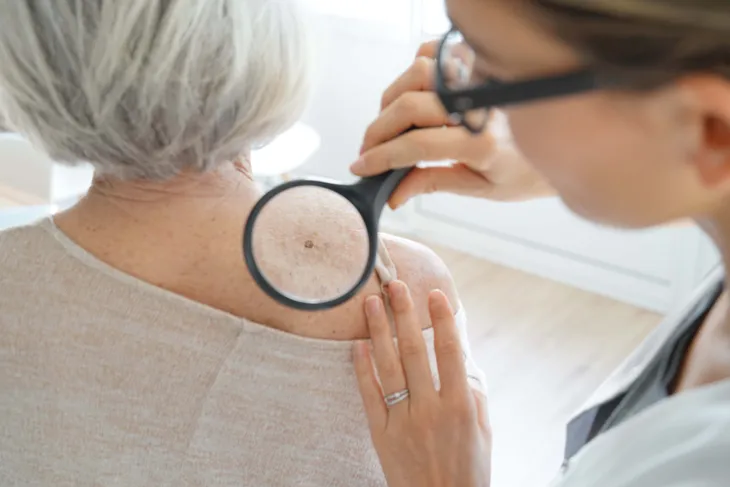
12. Dark Spots on the Skin
Keeping a watchful eye on any changes to our skin is something we should all get in the habit of, particularly when concerning skin cancer. But there’s also another reason we should be watching our skin closely. Dark spots on the skin which often appear on the neck, under the armpits, or even in the groin area, are a common early warning sign that a person is resistant to the hormone that regulates glucose in the blood, which is a “precursor to diabetes — the medical name for the condition is acanthosis nigricans (AN),” writes Women’s Health.
“We see this often in women with polycystic ovary syndrome (PCOS),” says Dr. Kellis to the source. Women who suffer from PCOS are at a higher risk of developing diabetes and are often found to have issues with the hormone that regulates glucose in the blood. Keep an eye out for any dark spots on your skin, and if any are found, consult your doctor.
13. Feeling Itchy
There are many reasons that our skin can begin to feel itchy, but when it comes to diabetes, it is often due to dry skin, poor circulation, or even yeast infections, which surprisingly, can also occur on the skin, says the American Diabetes Association. You’ll know if the itching is the result of poor circulation because the itching will be localized to the legs, notes Women’s Health.
According to Health.com, the itchiness could also be from fluid loss due to frequent urination, “plus poor circulation and nerve damage due to thick, sugary blood can dry out your skin, especially on your lower extremities.”
The American Diabetes Association suggests people with diabetes who are suffering from itchiness to limit their bathing time, particularly in less humid climates. You should also use soap that contains moisturizer and apply moisturizer immediately after bathing.
14. Gum Disease
Inflamed or infected gums can be another strange sign of type 2 diabetes, according to Health.com. While these symptoms are actually a sign of gum disease, often referred to as periodontitis, research published in the journal BMJ Open Diabetes Research & Care found that it can also be linked to type 2 diabetes. “The study found that people with gum disease, especially those with severe cases, had higher rates of diabetes (both diagnosed and undiagnosed) and pre-diabetes than those without),” writes Health.com.
The connection between diabetes and gum disease can go both ways, as they could both equally be responsible for causing the other. In other words, both increase the risk of developing the other. “Inflammation caused by gum disease eggs on the same factors that are responsible for high blood sugar that cause diabetes,” says Ronald Tamler, MD, director of the Mount Sinai Clinical Diabetes Institute, to Health.com.
15. Emergency Symptoms of Type 2 Diabetes
Now that we’ve listed all the early warning signs and most common symptoms of type 2 diabetes, let’s talk about some of the emergency symptoms. Diabetes is a serious condition, as high blood sugar can cause long-term damage to the body. At the same time, so can low blood sugar, also known as hypoglycemia. “For people with type 2 diabetes, only those who are on medications that increase the body’s [hormone that regulates glucose in the blood] levels are at risk for low blood sugar,” writes Healthline.
The source goes on to list the emergency symptoms, or hypoglycemia symptoms, of type 2 diabetes which include, “shaking, dizziness, hunger, headache, sweating, trouble thinking, irritability or moodiness,” and “rapid heartbeat.” Any diabetic who is on medication that can lower their blood sugar should know how to treat the symptoms associated with hypoglycemia, says the source.