Over 25 million people in the U.S. have type 2 diabetes; however, the majority of individuals with diabetes are not aware they have the condition due to the fact that the symptoms, seem more like annoyances than signs of a dangerous condition. It is always important to know the most common symptoms in order to be better aware of any conditions you might be facing.
Here are the 20 most common symptoms of type 2 diabetes…
1. Numbness
Numbness that starts as a tingling in the hands, fingers, legs, and feet is often an early warning sign of diabetes. This occurs due to an increase in blood sugar levels, causing decreased blood flow to the extremities; and eventually damage to nerve fibers. For many, this numbness is often the first sign of any health issues.
Numbness from diabetes usually presents as a prickly, tingling, or painful sensation in the hands and feet that starts out minor at first, but as the nerve damage progresses over time, (and sometimes years), mild tingling can become chronic and quite painful, involving motor and sensory function as well as autonomic and involuntary nervous system responses with sudden and painful numbness in the fingers, toes, feet, hands, legs, and arms, which is sometimes accompanied by muscle wasting of the hands and feet.
2. Increased Urination
Typically, diabetes sufferers claim they have an overwhelming urge to urinate, and when they do urinate, the amount is quite significant. This increased urination is what often spurs a doctor’s visit and diagnosis of type 2 diabetes. This increased urination will often result in severe dehydration. So, it’s vital to maintain adequate. If the body becomes dehydrated, immune function decreases, leaving you susceptible to all sorts of illnesses and even damage to kidney function.
Polyuria is the term doctors use to refer to increased urination. It is a condition that causes the output of urine to increase above normal and passing abnormally large amounts of urine (typically more than 3 liters per day as compared to the average of 1 to 2 liters per day) each time you go to the bathroom. Polyuria is a common symptom of type 2 diabetes (and also type 1 diabetes).
3. Weight Loss
Rapid and unexplained weight loss is common with diabetes, because the body can’t absorb glucose (sugar) properly. This occurs with unmanaged type 1 diabetes in particular. However, patients with undiagnosed type 2 diabetes can also experience considerable and sudden weight loss with no obvious cause (i.e., no exercise or dietary changes).
When your body’s hormone levels aren’t regulated, it will begin to burn fat and muscle as a source of energy. Obviously, this will reduce overall body weight. If you have suddenly and unintentionally shed between 5 and 10 pounds of body weight in less than 6 months, talk to your doctor immediately. Your doctor can conduct a blood test to determine if you have diabetes and begin treatment immediately to manage your blood sugar levels.
4. Increase in Appetite
An increase in appetite often comes with sudden weight loss, which may make you feel fortunate at first because you feel like you can eat anything you want without consequences. However, your body is in a diabetic state, robbing your cells of essential energy, which explains the increased hunger that often isn’t satiated for long after eating a meal.
Increased appetite and the consumption of more calories than your body requires for energy expenditure may lead to weight gain. It’s normal to have an increased appetite after physical exertion, but this is generally alleviated after eating. However, a significantly increased appetite over a prolonged period could be a symptom of a serious illness, such as diabetes or hyperthyroidism. If you are experiencing excessive hunger that is ongoing, make an appointment to see your doctor.
5. Blurry Vision
You may already know that diabetes can lead to vision issues and even blindness if left untreated. It’s true that blurred vision is a common symptom of type 2 diabetes. This occurs as glucose levels spike, damaging blood vessels and restricting the flow of fluid to the eyes. If a diabetes diagnosis isn’t made, the patient could suffer complete vision loss. According to the American Diabetes Association, diabetes patients are at higher risk for minor eye disorders and blindness as compared to those without the disease. This is why regular eye exams are important.
Diabetes patients also have a 40-percent higher risk of developing glaucoma (a condition that causes increased pressure in the eye and retinal nerve damage) as compared to non-diabetic individuals. Statistics from the American Diabetes Association claim that the longer a patient has diabetes, the higher the risk of glaucoma. Likewise, the risk of cataracts (clouding over of the eye’s lens) is 60-percent higher in patients with diabetes.
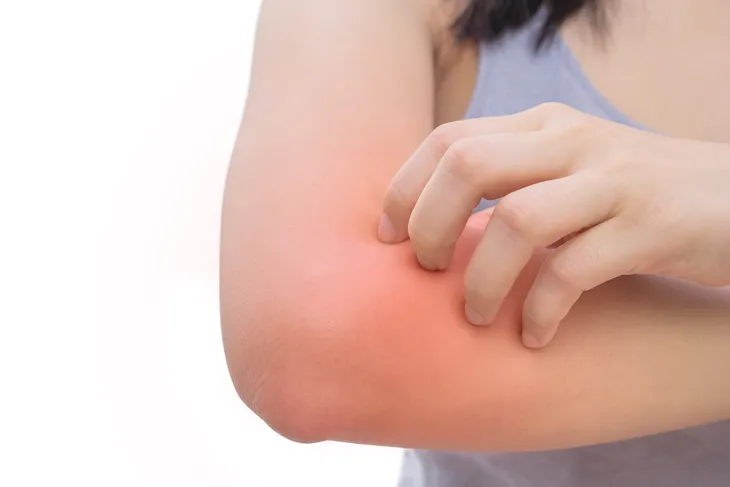
6. Itchy, Dry Skin
Type 2 diabetes can affect every part of the body, including the skin. When diabetes affects blood circulation, our sweat glands will often become dysfunctional, resulting in dehydrated, flaky, itchy, and irritated skin. This is why skin issues are often the first sign of a problem and the first indication of diabetes. Luckily, management of diabetes means that most skin conditions can be prevented and cleared up once caught early.
Undiagnosed diabetes patients are more prone to several skin ailments, including diabetic dermopathy, fungal infections, diabetic blisters, bacterial infections, dry and itchy skin due to poor circulation in the lower parts of the legs, necrobiosis lipoidica diabeticorum, boils, carbuncles, eruptive xanthomatosis, and fingernail and toenail infections.
7. Unexplained Fatigue
Fatigue is one of the most prevalent and frustrating symptoms of diabetes. Sudden fatigue can disrupt every aspect of your life (e.g., social, career, family life). Even hobbies that you were once passionate about may suddenly be ignored, because you just don’t have adequate energy.
When blood glucose is high, as it is with type 2 diabetes, your blood can become thick and “sludgy,” resulting in decreased circulation that prevents the transport of vital nutrients and oxygen to cells. This can also occur when blood sugars are low and fuel is not adequate to energize the body. Many people with type 2 diabetes also suffer from extreme exhaustion due to inflammation of the blood vessels.
8. Unquenchable Thirst
We’ve already established that type 2 diabetes can cause increased urination, both in frequency and amount of urine purged from the body with each bathroom break. The increased urge to urinate will rapidly lead to a state of dehydration. The body will demand that lost liquid be replenished, and an unquenchable thirst will often result as a direct effect of these lost body fluids.
However, diabetics can also become extremely thirsty for other reasons. For instance, high blood sugar levels can cause dry mouth, dehydration, and increased thirst in those with undiagnosed diabetes. Once blood sugar is controlled managed, thirst will generally return to normal. A condition known as diabetes insipidus, which impacts the kidneys via hormones, can also cause an increase in urination, dehydration, and increased thirst.
9. Slow Healing Cuts or Bruises
You might notice that healing takes much longer than normal if you suffer a cut or bruise. Wounds, burns, abrasions, or sores that take more than a few weeks to heal are prone to infection and often require medical treatment, which can indicate an underlying health issue such as undiagnosed diabetes. This slow healing is due to high blood glucose levels weakening the immune system and slowing the rate of healing.
This is also due to high blood glucose levels gradually damaging the nerves. Neuropathy (“disease of nerves”) can lead to poor blood circulation over time, impeding the transport of fresh blood for skin healing. In the case of burns, sores, and wounds that go unhealed for long durations, fungal and bacterial infections and eventually gangrene can develop.
10. Irritated Gums
Oftentimes, type 2 diabetes sufferers notice that their gums become red, swollen, and irritated. They might also literally see the gums receding from the teeth and experience gum infections, eventually resulting in gum disease. According to researchers at Marquette University, periodontal disease (gum disease) and diabetes can actually feed off one another, causing more severe forms of each condition. This means that gum disease contributes to diabetes and vice versa.
Research from the American Academy of Periodontology (AAP) shows that unmanaged diabetes patients are particularly at risk for periodontal disease. The reasoning is that both gum disease and diabetes encourage inflammation throughout the entire body, and if you consider inflammation of essential body parts, such as blood vessels, inflammation can result in all sorts of issues, including stroke, kidney disease, heart disease, and more.
11. Dry Mouth
Dry mouth is another symptom of type 2 diabetes. In fact, it’s considered one of the most common and can affect those with type 1 diabetes as well. Although the exact reasons it occurs are unknown, it is believed that high blood sugar levels could be one of the culprits. Other potential causes may include dehydration (as a result of the unquenchable thirst mentioned earlier) and some medications that are used to treat diabetes.
How do you know if you have dry mouth? In addition to a reduced amount of saliva, Healthline.com indicates that common symptoms include “a rough, dry tongue,” “cracked and chapped lips,” and “difficulty with swallowing, talking, or chewing.”
12. Frequent Yeast Infections
While many women experience yeast infections (medically referred to as candidiasis), frequent recurrences may be indicative of type 2 diabetes. According to Everyday Health, this is especially the case in women whose “blood sugar levels are higher than normal.”
Although it’s not entirely clear what the connection is between high blood sugar and yeast infections, the source says, “Yeast gets energy from sugar, so in an environment that is moist with sugar, yeast may overgrow,” leading to infection. Since diabetes suppresses the immune system, it may be challenging to get rid of a yeast infection once it has begun.
13. Dark Patches of Skin
The dryness and itchiness mentioned earlier aren’t the only skin problems that can affect those with type 2 diabetes. In some cases, the Mayo Clinic says that “patches of dark, velvety skin in the folds and creases of their bodies” may develop, especially on the back of the neck, in the armpits, or on the elbows and knees.
This condition is known as acanthosis nigricans, and is most often indicative of too much of the hormone that regulates glucose in the blood. In those with diabetes, high levels tend to occur because they’ve developed resistance, where the body can’t use the glucose the body is creating. This leads to a buildup that “causes normal skin cells to reproduce at a rapid rate,” resulting in the appearance of dark patches of skin.
14. Erectile Dysfunction
In men, type 2 diabetes may cause troubles getting or maintaining an erection, which is also known as erectile dysfunction (ED). Although these two conditions may seem unrelated, Healthline says, “They tend to go hand-in-hand,” as those who have diabetes “are two to three times more likely to develop ED.”
So what’s the connection? The source says it’s because having elevated blood sugar levels can cause damage to the circulatory and nervous systems and damage to blood vessels and nerves “can impede a man’s ability to achieve an erection firm enough to have sexual intercourse.”
15. Frequent or Recurring Infections
Experiencing frequent or recurring infections is another red flag for type 2 diabetes. Bladder infections, in particular, are especially common among diabetics, due to elevated blood sugar levels. People with diabetes don’t always experience the pain associated with bladder infections, resulting in them not realizing there’s a problem until the infection has spread to the kidneys.
Foot infections are also common in diabetics, as Everyday Health reports that type 2 diabetes “can damage the architecture of the foot, including the skin, blood vessels, and nerves.” These infections tend not to present themselves until the disease has progressed to an advanced state.
16. Headaches
One of the most common sources of pain humans experience are headaches. While they can appear due to many health reasons, headaches can also be an indicator of type 2 diabetes. A headache itself isn’t necessarily harmful, but it does become a concern when you’re experiencing them frequently. Healthline says they occur in diabetics when their blood sugar is too high or too low.
People with diabetes have a greater chance of developing headaches than people without the condition. It can occur when your blood sugar gets too high (called hyperglycemia) or when your blood sugar gets too low (called hypoglycemia). The best way for diabetics to reduce the number of headaches they get is by keeping track of their blood glucose.
 Syda Productions / Shutterstock
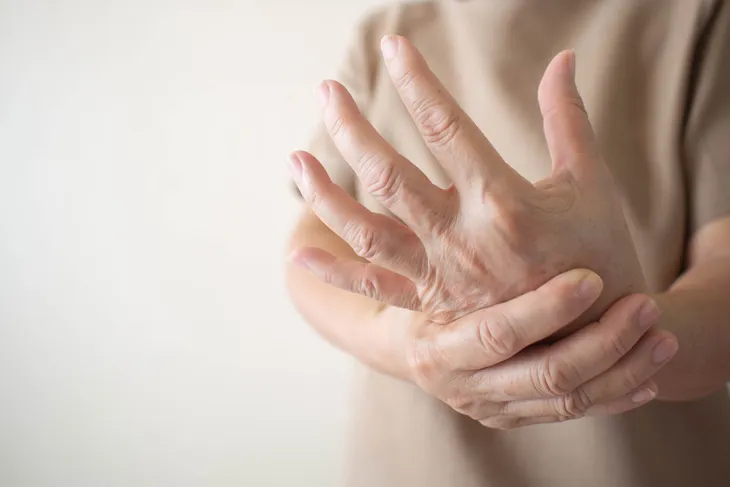
Syda Productions / Shutterstock17. Nerve Damage
Some people with type 2 diabetes will experience nerve damage. This condition is formally known as diabetic neuropathy and is likely caused by high blood sugar levels. It’s a common symptom that can impact up to 50 percent of diabetics, according to Mayo Clinic.
There are different types of diabetic neuropathy. Most people will feel tingling, pain, or numbness in the hands and feet. But it can also occur in other parts of the body such as the stomach, bowels, bladder, genitals, or even the heart.
 Orawan Pattarawimonchai / Shutterstock
Orawan Pattarawimonchai / Shutterstock18. Loss of Consciousness
People with type 2 diabetes may feel faint, dizzy, or completely lose consciousness. This is likely due to a condition called hypoglycemia. It occurs when blood sugar levels drop too low. Severe drops in blood sugar can make you pass out.
The only way to know whether these symptoms are due to hypoglycemia is by getting your blood sugar tested. Those already diagnosed with type 2 diabetes can also experience this symptom as a result of taking certain medications to manage their condition.
 Tunatura / Shutterstock
Tunatura / Shutterstock19. Diabetic Ketoacidosis
One complication people with type 2 diabetes may develop is diabetic ketoacidosis. This occurs when the body can’t produce enough insulin. Diabetic ketoacidosis has its own list of symptoms and warning signs. It can also be one of the first indicators that a person has diabetes.
Symptoms for diabetic ketoacidosis can develop fast. Some of them include:
- Excessive thirst
- Nausea
- Stomach pain
- Shortness of breath
- High blood sugar level
- High ketone levels in urine
You can find out more specific information about diabetic ketoacidosis by searching online.
 Vitalii Vodolazskyi / Shutterstock
Vitalii Vodolazskyi / Shutterstock20. Some People May Not Have Symptoms At First
While there are many symptoms related to type 2 diabetes, it’s possible for people not to experience symptoms at all. Type 2 diabetes develops slowly over time. This means some people might not experience noticeable symptoms for years.
The best way to monitor any changes in your health by getting regular check ups with your doctor. Since anyone can develop type 2 diabetes, you should also find out whether you carry any risk factors. This will help you better understand your chances of developing this disease.